Program for transplant patients hold old hearts in hands, offering a comprehensive guide to the journey of organ transplantation. This program delves into the multifaceted aspects of this life-altering experience, from the initial support systems and medical procedures to the long-term health implications and emotional challenges.
The program explores the intricate process of organ transplantation, covering everything from evaluation and selection to post-transplant care. It also addresses the often-overlooked emotional and psychological impact on patients, providing insights into coping mechanisms and the role of mental health professionals. Financial and practical challenges are also examined, including insurance, financial aid, and adjustments to daily life. The program also delves into ethical considerations, including informed consent and organ allocation.
This holistic approach aims to empower patients and their families with the knowledge and support they need to navigate this transformative journey.
Patient Support and Resources: Program For Transplant Patients Hold Old Hearts In Hands
Navigating the complexities of organ transplantation can be emotionally and physically challenging for patients and their families. A robust support system is crucial for successful recovery and long-term well-being. This section explores the various resources available to transplant recipients, highlighting the importance of community, family, and professional support.Comprehensive support is essential for transplant patients, extending beyond the immediate medical care.
This includes emotional, psychological, and practical assistance. Recognizing the diverse needs of this population, it’s important to understand the varying support structures available.
These programs for transplant patients, holding those old hearts in their hands, are truly inspiring. It’s a testament to the human spirit. But think about how your lifestyle choices, like giving up fast food, might impact your overall health, including your fertility. Check out this helpful article on boost your fertility give up fast food for some great tips.
Ultimately, these programs are about fostering a healthy lifestyle, inside and out, for the long haul, just like these incredible transplant patients.
Support Systems Available for Transplant Patients
A strong support system is critical for transplant patients. It encompasses various facets, including medical professionals, community organizations, family, and friends. The interconnectedness of these elements fosters a supportive environment conducive to recovery and long-term adjustment.
- Medical Professionals: Transplant teams play a pivotal role, providing ongoing medical care, monitoring, and education. These teams often include physicians, nurses, social workers, and psychologists. Their expertise and guidance are invaluable throughout the entire transplant journey.
- Community-Based Programs: Many communities offer specialized programs and support groups designed specifically for transplant recipients. These programs offer a unique opportunity for patients to connect with others facing similar experiences. Examples include workshops on managing medications, coping strategies, and navigating post-transplant life. These programs often provide valuable peer support and practical advice.
- Family and Social Networks: The role of family and social networks cannot be overstated. Strong family and social connections can provide emotional support, practical assistance, and a sense of belonging. This support network can be instrumental in helping patients adjust to the changes brought about by transplantation. Open communication and mutual understanding within the family unit are vital.
Resources for Emotional and Psychological Support
The emotional and psychological toll of transplantation can be significant. Addressing these needs is crucial for a positive recovery trajectory. A multi-faceted approach, incorporating various support resources, is often necessary.
- Mental Health Professionals: Psychologists, psychiatrists, and counselors can provide specialized support for transplant patients. They can help patients process their emotions, cope with stress, and address any psychological challenges that may arise. These professionals can help patients develop healthy coping mechanisms.
- Support Groups: Support groups offer a safe and confidential space for transplant recipients to share their experiences, connect with others facing similar challenges, and gain valuable insights from their peers. These groups provide a sense of community and understanding.
- Therapeutic Interventions: Various therapeutic interventions, such as cognitive behavioral therapy (CBT), can be beneficial in managing stress, anxiety, and depression. These techniques can empower patients to develop effective coping strategies for dealing with the challenges of transplantation.
Types of Support Groups and Their Benefits
Different types of support groups cater to specific needs and preferences. The table below Artikels various options and their associated advantages.
| Type of Support Group | Benefits |
|---|---|
| Patient-to-Patient Support Groups | Sharing experiences, developing a sense of community, gaining support and advice from peers, fostering mutual understanding. |
| Family Support Groups | Providing support to families of transplant recipients, offering a space for emotional processing and shared experiences, improving communication and understanding. |
| Online Support Forums | Accessibility from anywhere, anonymity, 24/7 support, connecting with a wider network of recipients and families. |
| Support Groups Facilitated by Professionals | Guidance from trained professionals, structured support, personalized support tailored to specific needs, addressing unique psychological challenges. |
Medical Procedures and Protocols
Navigating the world of organ transplantation requires understanding the intricate medical procedures and protocols involved. From the initial evaluation to the long-term recovery, each step is crucial for a successful outcome. This journey often involves significant emotional and physical challenges for both the recipient and the donor family. It is a testament to human resilience and medical innovation.The meticulous process of organ transplantation encompasses a series of steps designed to maximize the chances of success and minimize risks.
This includes a rigorous evaluation of potential candidates to ensure their suitability for the procedure. Furthermore, post-transplant care is a multifaceted approach encompassing medication management, regular check-ups, and adherence to a strict lifestyle regimen.
Evaluation and Selection Process
The evaluation process for transplant candidates is a multi-faceted approach. Potential recipients undergo extensive medical assessments to determine their overall health, the severity of their condition, and their suitability for transplantation. Factors considered include the patient’s overall medical history, the specific organ failing, and their capacity to manage the demanding post-transplant care regimen. This assessment process ensures that candidates are well-matched with suitable donor organs, increasing the chances of a positive outcome.
Detailed imaging studies, blood tests, and other diagnostic procedures provide critical information about the patient’s physical condition and identify any underlying health concerns.
Organ Procurement and Preservation
Organ procurement is a delicate and time-sensitive process. Once a suitable donor organ is identified, the organ procurement team swiftly removes it from the donor’s body and transports it to the recipient’s hospital. Preservation techniques are crucial in maintaining the viability of the organ during transport. These techniques employ specialized solutions and protocols to minimize organ damage and preserve its functionality.
Surgical Procedure
The surgical procedure for organ transplantation is highly complex. It involves the meticulous removal of the diseased organ from the recipient and the careful implantation of the donor organ. Surgeons meticulously stitch the new organ into place, ensuring proper blood supply and function. The surgery itself is a complex procedure, requiring a skilled surgical team and the latest medical technology.
Post-transplant Care
Post-transplant care is a multifaceted and long-term commitment. Recipients require ongoing medical support to manage potential complications and ensure the long-term success of the transplant. This includes taking immunosuppressant medications to prevent organ rejection, regular monitoring for complications, and adhering to strict dietary and lifestyle recommendations.
Programs for transplant patients, holding those old hearts in their hands, are truly remarkable. Imagine the profound impact on a recipient’s life, similar to navigating the complexities of life after a major health event, like a stroke. Reading about someone’s experience living for 15 years after a stroke offers invaluable insight into the resilience of the human spirit what its like to live for 15 years after a stroke.
It’s a reminder that these transplant programs not only offer a new lease on life, but also a chance to embrace the present and forge a new path, even with the scars of the past.
Phases of Recovery
The recovery process following a transplant is typically organized into distinct phases:
- Initial Post-operative Phase: This phase focuses on stabilizing the patient after surgery, closely monitoring vital signs and potential complications. This involves frequent assessments, medication management, and monitoring for signs of infection or rejection.
- Early Recovery Phase: During this phase, the patient begins to regain strength and mobility, gradually increasing their activity levels. This period also involves ongoing monitoring of organ function and medication adjustments.
- Long-term Recovery Phase: This phase focuses on the long-term management of the transplant, including ongoing medication, regular check-ups, and lifestyle modifications to maintain optimal health and prevent organ rejection. This phase emphasizes preventative measures to minimize the risk of complications and to optimize the long-term success of the transplant.
Comparison of Organ Transplant Procedures
| Organ Transplant | Surgical Complexity | Post-transplant Challenges | Success Rate (estimated) |
|---|---|---|---|
| Kidney | Relatively less complex | Risk of infection, hypertension, and chronic kidney disease | High (over 90%) |
| Liver | Highly complex | Risk of rejection, liver failure, and infections | Moderately High (around 80%) |
| Heart | Extremely complex | Risk of rejection, infections, and cardiovascular complications | High (over 85%) |
| Lung | Complex | Risk of rejection, infections, and respiratory complications | Moderately High (around 75%) |
Long-Term Health Implications
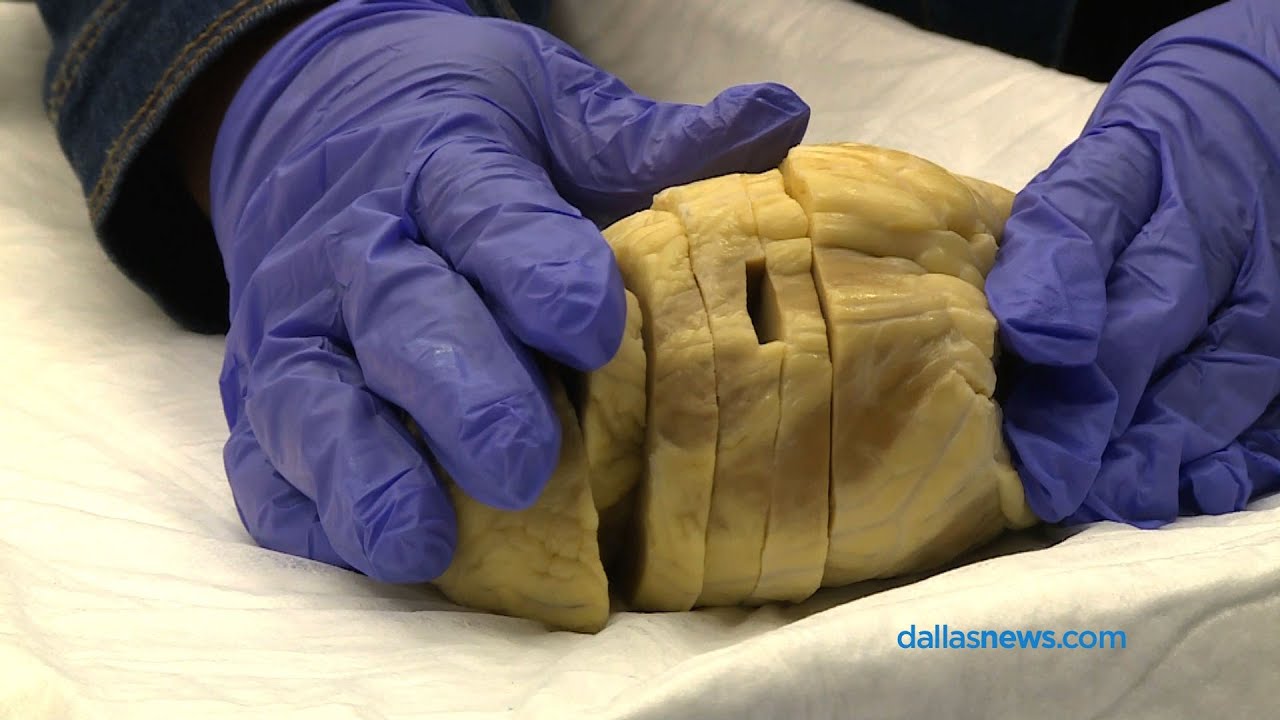
Living with a transplanted organ is a significant life change. Beyond the initial recovery period, transplant recipients face a range of long-term physical and mental health considerations. This phase requires careful management, ongoing medical attention, and a proactive approach to maintaining overall well-being. The long-term effects are multifaceted and require understanding to navigate successfully.The long-term health of a transplant recipient is significantly influenced by the immune system’s response to the new organ.
The body’s natural defense mechanisms must be carefully managed to prevent rejection. This necessitates a lifelong commitment to medication and regular medical check-ups. The focus shifts from acute recovery to proactive health maintenance.
Long-Term Physical Effects
Managing the long-term physical effects of organ transplantation involves meticulous attention to the effects of immunosuppressant drugs, alongside careful monitoring for potential complications. These drugs, while essential for preventing rejection, can have side effects that impact various bodily systems. Monitoring blood pressure, kidney function, and blood sugar levels is critical. The risk of developing infections is also elevated due to the immunosuppressed state.
Maintaining a healthy lifestyle, including a balanced diet and regular exercise, is vital for managing these effects and improving overall quality of life.
Long-Term Mental Well-being, Program for transplant patients hold old hearts in hands
The emotional toll of organ transplantation can be substantial. The physical challenges, the ongoing medical regimen, and the potential for complications can lead to stress, anxiety, and depression. Addressing these mental health concerns is crucial for a successful long-term outcome. Support groups, counseling, and open communication with healthcare providers are vital resources for patients and their families.
Understanding the psychological adjustments required is essential for positive mental well-being.
Importance of Ongoing Medical Follow-up and Management
Regular medical check-ups are essential for monitoring the health of the transplanted organ and the recipient’s overall well-being. These appointments provide opportunities to detect and address any emerging issues promptly. Early intervention can often prevent complications from escalating. A close relationship with a dedicated healthcare team is crucial for navigating the complexities of long-term care.
Potential Complications and Management Strategies
Various complications can arise post-transplant. These can range from infections to organ damage. One example is the development of kidney disease, often a consequence of long-term immunosuppressant use. A multi-disciplinary approach, involving nephrologists and other specialists, is critical for managing such complications effectively. Prompt diagnosis and treatment are key to mitigating the impact of these challenges.
Adherence to Medication Regimens
Adherence to the prescribed medication regimen is paramount for long-term success. This includes taking medications as directed and at the appropriate times. Immunosuppressant medications are crucial for preventing rejection, and consistent use is essential. The consequences of missing doses can be significant, potentially leading to organ rejection or other complications. Educating patients about the importance of adherence and providing support mechanisms are critical for successful outcomes.
Potential Long-Term Side Effects of Immunosuppressant Medications
| Medication Category | Potential Side Effects |
|---|---|
| Calcineurin Inhibitors (e.g., cyclosporine, tacrolimus) | Nephrotoxicity (kidney damage), hypertension (high blood pressure), tremor, hirsutism (excessive hair growth), hyperkalemia (high potassium levels), gum hyperplasia (gum overgrowth) |
| Mycophenolate Mofetil (MMF) | Gastrointestinal upset (nausea, vomiting, diarrhea), headache, fatigue, liver problems |
| Corticosteroids (e.g., prednisone) | Fluid retention, osteoporosis (bone loss), hyperglycemia (high blood sugar), weight gain, mood changes, increased risk of infections |
| Anti-rejection antibodies | Increased risk of blood clots, various side effects depending on the specific medication |
Financial and Practical Challenges
The journey of organ transplantation, while offering a lifeline, often comes with significant financial and practical burdens. Navigating these challenges can be emotionally and logistically demanding for both the transplant recipient and their family. This section explores the multifaceted financial strain and the practical adjustments required for a successful transition into a new phase of life.
Financial Burdens Associated with Transplantation
The costs associated with transplantation extend far beyond the initial surgery. Pre-transplant evaluations, medications, and post-operative care contribute to a substantial financial burden. Many individuals face significant out-of-pocket expenses, including travel, lodging, and lost wages due to time off work for procedures and recovery. The emotional and physical toll of the illness leading to the transplant also impacts the patient’s ability to work, adding to the financial strain.
Some pre-transplant medical expenses may not be covered by insurance, increasing the financial burden on the patient.
Accessing Healthcare Insurance and Financial Aid
Insurance coverage for organ transplantation varies significantly depending on the individual’s policy and the specific procedures involved. Navigating the intricacies of insurance claims and appeals can be challenging. Financial aid programs and resources are available to help transplant patients manage these costs. These programs often provide assistance with medications, travel, and other related expenses. The patient should thoroughly research and apply for any available financial aid programs to alleviate the financial strain.
This proactive approach can greatly ease the financial stress associated with the transplant.
Programs for transplant patients, holding old hearts in hands, are truly inspiring. Seeing actors like those from “Stranger Things” use their platform to raise awareness for rare diseases, like in this recent article about a specific case netflix stranger things actor puts positive spotlight on rare disease , is a powerful reminder of the human connection and hope these programs offer.
It highlights the importance of support and advocacy for these incredible individuals undergoing such life-altering procedures.
Practical Challenges Faced by Transplant Patients and Families
Post-transplant life presents unique practical challenges. The need for frequent medical appointments, medication management, and potential lifestyle adjustments can impact daily routines. Travel to medical facilities, adherence to strict medication schedules, and the need for supportive care from family members or caregivers significantly affect daily life. For families, adjusting their work schedules and personal commitments to support the transplant recipient can also be a significant challenge.
These practical difficulties can lead to stress and emotional strain, so understanding and support are crucial.
Housing and Employment Adjustments
The need for ongoing medical care and potential physical limitations post-transplant may necessitate adjustments to housing and employment situations. Individuals may require accessible housing with appropriate support systems, or need to relocate closer to medical facilities for easier access to appointments. The unpredictable nature of post-transplant health can also impact employment. Individuals may need to reduce work hours, find flexible employment options, or take time off work for appointments and recovery.
Understanding these needs and exploring options early on is vital.
Cost of Immunosuppressant Medications
Immunosuppressant medications are essential for preventing organ rejection after transplantation. However, these medications can be expensive. The lifelong nature of these treatments necessitates a commitment to long-term financial planning. The costs of these medications can vary depending on the specific medication and the dosage required. Many insurance plans cover immunosuppressants, but patients should confirm coverage with their providers.
Some financial aid programs may provide partial or full assistance with these costs.
“The long-term financial commitment of immunosuppressant medications should be a major consideration during the decision-making process.”
Careful budgeting and exploring financial aid programs are vital for managing the costs of immunosuppressant medications.
Emotional and Psychological Well-being
The journey of organ transplantation is profoundly impactful, extending far beyond the physical recovery. Navigating the emotional and psychological adjustments is crucial for successful long-term outcomes. The anticipation, the surgery, the recovery, and the ongoing management all contribute to a complex emotional landscape that requires careful attention and support.The experience of organ transplantation can trigger a wide range of emotions, from overwhelming gratitude and hope to anxiety, fear, and grief.
The physical trauma, the uncertainty about the future, and the potential for long-term health implications can all take a toll on mental well-being. This section delves into the emotional and psychological challenges faced by transplant recipients and offers strategies for coping.
Impact of Transplantation on Mental Health
Organ transplantation, while life-saving, significantly impacts a recipient’s psychological state. The process itself is demanding, requiring extensive medical procedures, lifestyle changes, and strict adherence to medication regimens. This often leads to feelings of stress and anxiety. The emotional toll can be further amplified by the anticipation, the uncertainty surrounding the outcome, and the fear of potential rejection.
Post-transplant, recipients may grapple with adjustment issues, worries about long-term health, and the need to manage medication side effects.
Potential for Anxiety, Depression, and Stress
Anxiety, depression, and stress are common experiences among transplant recipients. Anxiety may manifest as worry about rejection, complications, or the side effects of immunosuppressants. Depression can arise from the physical limitations, the challenges of adapting to a new lifestyle, or feelings of vulnerability. Stress, triggered by the demanding medical regimen and the fear of relapse, can also significantly impact emotional well-being.
In some cases, these conditions can become severe and require professional intervention.
Coping Mechanisms for Emotional Challenges
Developing healthy coping mechanisms is vital for managing the emotional challenges associated with organ transplantation. These include stress-reduction techniques like meditation, deep breathing exercises, and mindfulness. Building a strong support network, whether through family, friends, or support groups, can offer invaluable emotional comfort and guidance. Maintaining a positive outlook and focusing on personal strengths and accomplishments can also foster resilience and emotional stability.
Regular exercise and a balanced diet can also play a significant role in promoting emotional well-being.
Role of Mental Health Professionals
Mental health professionals, such as psychologists and psychiatrists, play a crucial role in the recovery process of transplant recipients. They can provide a safe space for expressing anxieties, fears, and concerns, offering guidance and support in developing coping strategies. They can help patients process their emotions, address any potential mental health conditions, and facilitate adaptation to the new life circumstances.
Psychotherapy and counseling can help individuals develop healthy coping mechanisms and build resilience. Medication, when appropriate, can also help manage symptoms of anxiety or depression.
Resources for Mental Health Support
- Support Groups: Support groups offer a crucial outlet for sharing experiences and connecting with others who understand the challenges of transplantation. These groups provide a sense of community and support, fostering emotional connection and resilience.
- Mental Health Professionals: Seeking guidance from licensed therapists, psychologists, or psychiatrists can offer personalized support and strategies for managing mental health concerns. They can tailor treatment plans to individual needs and circumstances.
- Online Forums: Online forums dedicated to transplant recipients can offer a platform for connecting with others, sharing experiences, and accessing information. This online support system can provide invaluable emotional support and a sense of community.
- Community Centers: Local community centers or hospitals often offer workshops and support groups for patients and their families. These resources can be invaluable for providing practical support and connecting individuals with the right resources.
Understanding the Journey
The transplant journey is a multifaceted and deeply personal experience, impacting every aspect of a patient’s life. From the initial diagnosis to the long-term care, the path is fraught with both challenges and triumphs. Navigating this complex process requires a strong support system and a profound understanding of the emotional and physical demands. This section delves into the patient’s experience throughout the process, providing a timeline, discussing challenges, and highlighting the significance of support networks.The transplantation journey is a marathon, not a sprint.
It encompasses a spectrum of emotions, from fear and anxiety to hope and gratitude. This journey is unique for each individual, but common threads of experience weave through the narrative. Understanding these threads can offer valuable insight and support for those navigating this complex path.
The Transplantation Timeline
The transplantation journey unfolds over a significant period, spanning from initial diagnosis to long-term care. Each phase presents unique challenges and opportunities for growth and resilience.
- Initial Diagnosis and Evaluation: This phase involves comprehensive medical evaluations to assess the patient’s suitability for transplantation. This period can be overwhelming, marked by uncertainty and fear. Doctors explain the procedure, potential risks, and the necessary steps involved. The patient begins to understand the severity of their condition and the potential for a new lease on life.
- Pre-transplant Preparation: This stage includes extensive medical preparation, such as blood tests, scans, and medication adjustments. The patient undergoes rigorous physical and psychological assessments to ensure they are fit for the procedure. This period is often a time of intense anticipation and stress.
- The Transplantation Procedure: This is the crucial moment. The transplantation surgery itself is a complex procedure. The emotional experience varies greatly. Some patients experience anxiety, while others feel a sense of profound hope. The team works diligently to ensure the patient’s safety and well-being.
- Post-transplant Recovery: Recovery involves intensive monitoring and treatment. The patient is vulnerable during this phase and may experience pain, discomfort, and side effects. This is a time of both physical and emotional healing.
- Long-Term Care: The journey continues after discharge. Patients need ongoing medical care, medication management, and regular check-ups. The focus shifts to managing long-term health implications and fostering a sustainable lifestyle.
Challenges and Triumphs
The transplantation journey is characterized by a spectrum of experiences. Patients face numerous challenges, but also find moments of triumph and resilience.
- Challenges: Challenges encompass physical discomfort, side effects from immunosuppressant medications, and the emotional burden of the process. Patients often experience anxiety, fear, and uncertainty about their future. They also need to adjust to a new lifestyle with ongoing medical needs.
- Triumphs: Triumphs are moments of joy, gratitude, and appreciation for the gift of life. They involve the patient’s ability to overcome adversity, adapt to new routines, and find strength in their support network. Experiencing positive health outcomes and the joy of being able to participate in daily life are examples of triumphs.
The Emotional Rollercoaster
The emotional experience of a transplant patient is complex and multifaceted. Patients experience a range of emotions that fluctuate throughout the entire journey.
- Fear and Anxiety: Fear and anxiety are common emotions during the pre-transplant and post-transplant phases. Uncertainty about the procedure’s outcome and the possibility of rejection or complications can create intense anxiety.
- Hope and Gratitude: Hope and gratitude are essential emotions that sustain patients throughout their journey. The prospect of a new life and the gift of another chance at health can foster profound hope and gratitude. Seeing improvements in health and regaining vitality are important emotional outcomes.
- Grief and Loss: The process can evoke feelings of grief and loss, as patients confront their old lives and embrace the new. Acceptance of the changes and understanding of the new reality are important parts of the process.
The Significance of Support Networks
A robust support network plays a critical role in a transplant patient’s journey. The emotional and practical support from family, friends, and support groups is indispensable.
- Family and Friends: Family and friends provide invaluable emotional support and practical assistance. They offer encouragement, understanding, and a listening ear during difficult times.
- Support Groups: Support groups provide a safe space for patients to connect with others who share similar experiences. These groups offer emotional support, practical advice, and a sense of community.
Ethical Considerations
Organ transplantation, a life-saving procedure, raises complex ethical questions that extend beyond the medical realm. Navigating these considerations requires careful thought, open dialogue, and a commitment to fairness and equity. From the initial decision to donate to the allocation of organs, ethical principles must guide every step of the process. This section explores the crucial ethical dimensions of organ transplantation.
Informed Consent and Patient Autonomy
The cornerstone of ethical organ transplantation is the principle of informed consent. Patients must fully understand the risks, benefits, and alternatives associated with the procedure, enabling them to make autonomous decisions about their health. This includes comprehending the potential short-term and long-term consequences of transplantation, as well as the impact on their overall quality of life. A critical aspect is ensuring the patient is mentally competent and capable of understanding the complexities involved, and that consent is voluntary, without coercion or undue influence.
This process safeguards the patient’s right to self-determination.
Ethical Dilemmas in Organ Donation and Transplantation
Organ donation and transplantation frequently present ethical dilemmas. One key challenge lies in balancing the needs of the recipient with the rights and wishes of the potential donor. Another is the allocation of scarce resources, such as organs. For example, a situation might arise where multiple patients require the same organ, requiring a prioritization system. Furthermore, concerns about the potential for exploitation or undue pressure on individuals to donate must be addressed.
Ethical guidelines must ensure that the process is transparent, fair, and respects the rights of all involved parties.
Organ Allocation and Prioritization
Organ allocation is a complex process that aims to ensure equitable distribution. Various criteria are used, including the patient’s medical urgency, the compatibility of the organ with the recipient, and the time elapsed since the organ became available. Different countries and regions have varying systems, but generally, these systems prioritize patients with the greatest need and the highest chance of survival.
This process must be transparent and publicly justifiable, with clear criteria for prioritization to minimize bias and promote fairness. One example is the use of waiting lists, which aims to manage the demand and ensure that organs are allocated based on need and time spent on the list.
Ethical Principles Governing Organ Transplantation
| Ethical Principle | Description |
|---|---|
| Beneficence | Acting in the best interests of the patient and promoting their well-being. |
| Non-maleficence | Minimizing harm to the patient and ensuring the procedure is performed with the highest standards of care. |
| Justice | Ensuring fair and equitable allocation of organs, preventing discrimination and promoting equal access. |
| Respect for Persons | Recognizing the inherent worth and autonomy of individuals involved in the process, including donors and recipients. |
This table Artikels the core ethical principles guiding organ transplantation. These principles provide a framework for navigating the complex decisions involved in this life-saving procedure. Understanding these principles helps ensure that the process is carried out ethically and with consideration for all parties.
Illustrative Case Studies
Navigating the complexities of organ transplantation is a deeply personal journey, and understanding individual experiences can offer valuable insights for patients, families, and healthcare professionals alike. Each case highlights the physical, emotional, and logistical challenges, as well as the remarkable resilience and hope that characterize this process. These stories demonstrate the wide range of outcomes and the importance of individualized support.
A Journey Through Heart Transplantation
The story of Amelia, a 48-year-old teacher diagnosed with end-stage heart failure, exemplifies the profound impact of transplantation. Amelia’s heart condition progressively worsened, leading to debilitating fatigue and shortness of breath. Her daily life was severely restricted, and the prospect of a normal life seemed distant. After months of rigorous testing and evaluation, Amelia was matched with a donor heart.
The surgery was successful, and Amelia experienced a gradual recovery. She faced challenges in managing medication, adhering to a strict post-operative diet, and maintaining physical activity. Amelia’s emotional well-being was also profoundly affected by the uncertainty of the transplant process. However, with consistent support from her family and the transplant team, she slowly regained her strength and joy.
Amelia returned to teaching, albeit with adjusted work hours, and found renewed purpose in her life.
Emotional Impact of Transplantation
The emotional toll of transplantation extends beyond the immediate post-operative period. Patients often experience a spectrum of emotions, from fear and anxiety to gratitude and hope. These emotions can significantly impact the patient’s overall well-being. For instance, the anticipation of the surgery, the uncertainty of the outcome, and the possibility of rejection can evoke significant emotional distress.
The psychological and emotional challenges may also vary according to the individual’s pre-existing conditions, family support, and personal coping mechanisms.
Positive Outcomes and Long-Term Success Stories
Transplantation offers a second chance at life for many individuals. Long-term success stories highlight the remarkable progress in medical technology and the resilience of transplant recipients. Patients often experience improved quality of life, enabling them to return to work, pursue hobbies, and engage in social activities. These positive outcomes often depend on meticulous post-transplant care, adherence to medication regimens, and proactive management of potential complications.
Regular check-ups, blood tests, and communication with the transplant team are crucial for maintaining health and longevity. Some patients, like David, a former athlete, returned to competitive sports after a successful liver transplant. The support and care he received played a critical role in his successful recovery and return to a fulfilling life.
Fictional Account of a Patient’s Journey
Imagine Sarah, a young mother with a rare genetic heart condition. Before the transplant, Sarah struggled with chronic pain, extreme fatigue, and the constant fear of sudden episodes. The uncertainty of her future weighed heavily on her and her family. The actual surgery was a blur of medical procedures and emotional turmoil. After the transplant, Sarah experienced a mix of elation and anxiety.
She had to adjust to a new life with a foreign heart and the need for lifelong medication. Initially, the physical recovery was challenging, marked by bouts of nausea and discomfort. The emotional challenges were equally significant, including moments of doubt and questioning the meaning of her life. However, with the support of her family, the medical team, and her newfound determination, Sarah eventually regained her health and found renewed purpose.
She now volunteers at a local hospital, sharing her story and inspiring others facing similar challenges.
Outcome Summary
In conclusion, the program for transplant patients hold old hearts in hands, offers a thorough and empathetic exploration of the complexities surrounding organ transplantation. By understanding the medical, emotional, and practical challenges, patients and their support networks can be better equipped to embrace the journey and achieve optimal outcomes. This program highlights the crucial role of support systems, medical expertise, and ethical considerations in ensuring the success and well-being of transplant recipients throughout their recovery and long-term lives.