With how to assess MS treatment at the forefront, this guide dives deep into the multifaceted world of evaluating MS treatment effectiveness. From defining key assessment criteria to understanding diverse patient populations, we’ll explore the crucial steps in monitoring treatment response and long-term management. This isn’t just about numbers; it’s about understanding the individual patient journey and tailoring assessments accordingly.
This in-depth exploration covers a range of topics, including different treatment types, their mechanisms of action, and common side effects. We’ll analyze the importance of patient adherence and education in achieving optimal treatment outcomes. Visual representations, such as graphs and charts, will illustrate treatment progress, while tables will organize key information for easy comprehension. The goal is to equip readers with the knowledge and tools needed to effectively assess MS treatment for their own or a loved one’s journey.
Defining Assessment Criteria
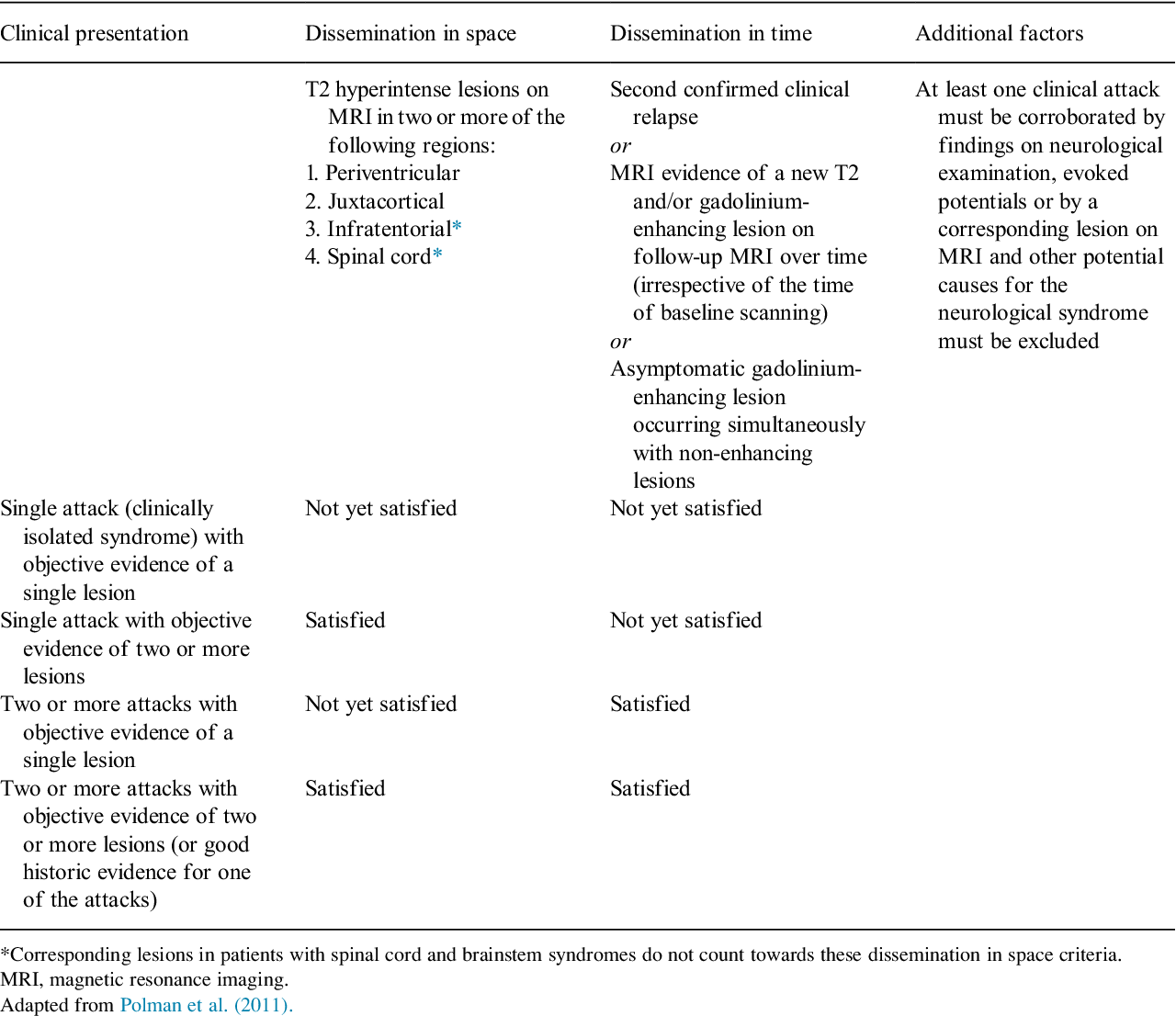
Evaluating MS treatment effectiveness requires a multifaceted approach, encompassing various factors that impact a patient’s well-being. This assessment isn’t a simple check-box exercise; rather, it demands a comprehensive understanding of how the treatment affects disease progression, disability, and overall quality of life. A detailed analysis of these factors allows clinicians to make informed decisions regarding treatment adjustments or modifications.
Key Factors in Assessing MS Treatment
Multiple sclerosis treatment effectiveness is evaluated using a combination of clinical observations and patient-reported outcomes. Different scales and measures are employed to quantify disease activity, disability progression, and quality of life. This ensures a holistic evaluation, providing a more complete picture of the treatment’s impact.
Disease Activity Metrics
Assessing disease activity is crucial in determining the effectiveness of MS treatments. These metrics measure the frequency and severity of relapses and new lesions, which indicate the inflammatory processes underlying MS. Several tools are employed to quantify these changes.
| Factor | Description | Measurement Method |
|---|---|---|
| Frequency of relapses | Number of exacerbations of symptoms over a defined period. | Clinical evaluation and documented symptom reports. |
| New brain MRI lesions | Detection of new or enlarging lesions on magnetic resonance imaging (MRI). | MRI scans at baseline and follow-up intervals, standardized lesion quantification. |
| Inflammatory markers | Blood tests measuring inflammatory components like cytokines or antibodies associated with MS. | Blood samples and laboratory analysis of inflammatory markers. |
| Clinical Disease Activity Scores | Composite scores summarizing various clinical manifestations of disease activity. | Multiple sclerosis functional composite (MSFC), expanded disability status scale (EDSS), or similar scales. |
Disability Progression Assessment
Monitoring disability progression is essential to evaluating treatment efficacy. This involves assessing the impact of MS on a patient’s functional abilities and daily activities.
| Factor | Description | Measurement Method |
|---|---|---|
| Expanded Disability Status Scale (EDSS) | Evaluates physical impairments, including walking ability, balance, and other motor functions. | Neurological examination and scoring system. |
| Multiple Sclerosis Functional Composite (MSFC) | Assesses several functional domains, including walking, cognition, and upper extremity function. | Standardized assessments of functional abilities. |
| Activities of Daily Living (ADLs) | Measures the patient’s capacity to perform basic self-care tasks, such as bathing, dressing, and eating. | Interview-based assessments or questionnaires. |
Quality of Life Assessment
Quality of life (QoL) is a crucial aspect of MS treatment evaluation, encompassing the patient’s emotional, social, and physical well-being.
Assessing MS treatment effectiveness can be tricky. It’s not just about medication; lifestyle choices play a huge role. Consider incorporating intense exercise like an olympian with this insider knowledge exercise like an olympian with this insider knowledge to boost your overall well-being, which can ultimately impact your MS symptoms. Tracking your energy levels, mood, and pain throughout the day is also vital in assessing the impact of any treatment.
| Factor | Description | Measurement Method |
|---|---|---|
| Patient Reported Outcome Measures (PROMs) | Questionnaires that gauge the patient’s perceptions of their health and well-being. | Specific questionnaires tailored to MS, such as the MSQoL-54, or the SF-36. |
| Emotional well-being | Assessment of mental health, mood, and stress levels. | Questionnaires, clinical interviews, or psychological assessments. |
| Social functioning | Evaluation of the patient’s ability to maintain relationships and participate in social activities. | Structured interviews, questionnaires, or observations. |
Types of MS Treatments
Multiple sclerosis (MS) treatment strategies encompass a diverse range of approaches, each aiming to manage the disease’s progression and alleviate its symptoms. Understanding the different types of treatments available is crucial for patients and healthcare providers in making informed decisions about the best course of action. This section explores the various treatment modalities, highlighting their mechanisms of action and potential side effects.Different treatment approaches target distinct aspects of MS, ranging from slowing disease progression to managing symptoms.
A personalized approach is essential, considering the individual patient’s needs and preferences.
Disease-Modifying Therapies (DMTs)
Disease-modifying therapies (DMTs) are a cornerstone of MS treatment. They aim to alter the course of the disease by reducing inflammation and slowing the progression of the disease. This is achieved through various mechanisms, including modulation of the immune system.
- Interferons (e.g., interferon beta-1a, interferon beta-1b): These medications interfere with the immune response, potentially slowing the development of new lesions in the central nervous system.
- Glatiramer acetate: This synthetic protein mimics myelin components, potentially reducing immune attack on myelin.
- Natalizumab: This monoclonal antibody targets a protein involved in immune cell migration, potentially reducing inflammation.
- Dimethyl fumarate: This medication is believed to have immunomodulatory effects, potentially reducing the frequency of relapses.
- Teriflunomide: This medication is thought to reduce the activity of the immune system, which might slow disease progression.
Symptomatic Therapies
Symptomatic therapies focus on managing the symptoms of MS, rather than addressing the underlying disease process. These therapies aim to improve quality of life by alleviating symptoms such as fatigue, pain, muscle spasms, bladder dysfunction, and depression.
- Muscle relaxants: Used to manage muscle spasms and stiffness. Examples include baclofen and tizanidine. However, muscle relaxants can lead to drowsiness and dizziness as side effects.
- Pain medications: These can help manage neuropathic pain, a common symptom of MS. Options include analgesics and antidepressants.
- Medications for bladder dysfunction: These address issues with bladder control, such as urgency and frequency. Examples include medications that increase bladder capacity or reduce spasms.
- Medications for depression: Depression is a common mental health concern in MS patients. Antidepressants are often prescribed to address this.
- Fatigue management strategies: These include lifestyle modifications, such as regular exercise and adequate sleep, as well as medications.
Complementary Therapies
Complementary therapies are non-pharmacological approaches that may offer some symptom relief. They are often used in conjunction with conventional therapies, but their efficacy in slowing disease progression is not consistently supported by robust scientific evidence.
- Physical therapy: This focuses on improving strength, balance, and coordination. It can be very helpful for patients experiencing mobility issues.
- Occupational therapy: This helps patients adapt their daily routines to manage their symptoms. It can involve assistive devices and training for specific tasks.
- Speech therapy: This is useful for patients with speech and swallowing difficulties.
- Nutritional counseling: A healthy diet and hydration are important for overall well-being.
- Mind-body therapies: Techniques like yoga and meditation can help manage stress and improve mood.
Comparison of Treatment Types
| Treatment Type | Target Symptoms | Potential Side Effects |
|---|---|---|
| Disease-Modifying Therapies (DMTs) | Slowing disease progression, reducing relapses, and preventing new lesions. | Flu-like symptoms, injection site reactions, liver problems (in some cases), and others. |
| Symptomatic Therapies | Managing specific symptoms such as pain, fatigue, muscle spasms, bladder dysfunction, and depression. | Drowsiness, dizziness, nausea, or other effects dependent on the specific medication. |
| Complementary Therapies | Symptom management, improving quality of life, and promoting well-being. | Generally considered safe, but potential interactions with other medications should be discussed with a physician. |
Evaluating Treatment Response
Navigating the complexities of multiple sclerosis (MS) treatment requires a keen understanding of how well the chosen therapies are working. This crucial aspect involves not just administering the treatment but also meticulously monitoring its impact on the disease’s progression and the patient’s overall well-being. Regular assessment is vital to adjust strategies and ensure the most effective course of action.
Frequency and Timing of Assessments
Understanding the appropriate frequency and timing of assessments is essential for evaluating MS treatment efficacy. This depends on the specific treatment, the patient’s individual response, and the nature of the symptoms being monitored. Frequent assessments are crucial in the initial stages of treatment to identify early responses or adverse effects. Regular check-ups help track progress and fine-tune the approach.
A personalized schedule, developed in consultation with the neurologist, ensures that assessments are both comprehensive and well-timed.
Parameters for Monitoring Treatment Efficacy
Various parameters need to be tracked to accurately evaluate treatment efficacy. These include clinical measures, neurological assessments, and patient-reported outcomes.
Assessing MS treatment effectiveness isn’t always straightforward. Factors like side effects and the rising cost of insulin play a huge role, which is why understanding the financial implications of treatment is crucial. For example, exploring resources like why is the cost of insulin rising and what can people do about it can help you navigate the challenges.
Ultimately, a holistic approach considering both medical and financial aspects is key to making informed decisions about your MS treatment plan.
- Clinical Measures: These objective measurements provide quantifiable data about disease activity. Examples include Expanded Disability Status Scale (EDSS) scores, which assess physical impairments, and MRI scans, which monitor lesions and brain atrophy. These measurements help track disease progression over time. Regular EDSS scores, coupled with MRI results, provide a clear picture of how the treatment is affecting the physical manifestations of MS.
- Neurological Assessments: These evaluations assess specific neurological functions, including strength, sensation, coordination, and reflexes. Specific tests may focus on the areas affected by MS. Examples of tests include visual evoked potentials (VEPs) for assessing optic nerve function, and electromyography (EMG) to monitor muscle function. These assessments aid in understanding the impact of treatment on the nervous system.
- Patient-Reported Outcomes (PROs): These measures focus on the patient’s subjective experience of MS symptoms and the impact of treatment. Questionnaires or scales designed to assess fatigue, cognitive impairment, and mood are crucial. This personal insight provides crucial context to objective measures.
Interpreting Assessment Results
Accurate interpretation of assessment results is critical to adjusting treatment strategies effectively. Comparing results over time reveals patterns that indicate treatment effectiveness or the need for adjustments. Understanding the baseline values and the specific changes observed is key. For example, a sustained decrease in EDSS scores alongside improvements in PROs suggest a positive treatment response.
Flowchart for Evaluating Treatment Response Over Time
The following flowchart illustrates the process of evaluating treatment response over time.
| Step | Action |
|---|---|
| 1 | Establish Baseline: Conduct initial assessments (EDSS, MRI, PROs). |
| 2 | Scheduled Assessments: Implement a regular assessment schedule (e.g., every 3 months). |
| 3 | Data Collection: Gather data from various assessment methods. |
| 4 | Data Analysis: Compare current results to baseline and previous assessments. |
| 5 | Interpretation: Assess treatment efficacy based on observed changes. |
| 6 | Adjustments: Modify treatment plan if necessary, based on observed patterns and recommendations. |
| 7 | Repeat: Repeat steps 2-6 as needed, maintaining a consistent schedule. |
Considerations for Diverse Patient Populations: How To Assess Ms Treatment
Assessing MS treatment effectiveness isn’t a one-size-fits-all process. Individual differences, including genetic predispositions, pre-existing health conditions, socioeconomic factors, and cultural backgrounds, significantly impact how a treatment manifests and is experienced. Recognizing these variations is crucial for tailoring assessment strategies and ensuring equitable access to effective therapies.Understanding the unique needs of diverse populations allows for more accurate evaluations of treatment efficacy and side effects, ultimately leading to better outcomes.
This involves adapting assessment tools and methodologies to address potential barriers and ensure that the process is sensitive and respectful of cultural norms and values.
Genetic Background Variations
Genetic variations can influence how individuals respond to MS treatments. Some genetic markers might predict a higher likelihood of side effects or a less favorable treatment response. Identifying these markers can help personalize treatment plans and potentially reduce adverse events. For example, specific genetic predispositions might impact the efficacy of disease-modifying therapies, leading to adjustments in dosage or treatment choice.
Clinicians should be aware of these potential variations and incorporate genetic information into treatment decisions.
Comorbidities and Their Impact
Patients with MS often have co-occurring conditions (comorbidities). These conditions can influence treatment effectiveness and necessitate adjustments to assessment strategies. For instance, patients with hypertension might require careful monitoring of blood pressure responses to treatments, as certain medications could exacerbate the condition. Assessing the impact of comorbidities requires careful consideration of potential interactions and adjustments to treatment protocols.
The presence of other medical conditions may influence the choice of MS therapies and the assessment of their efficacy. For example, a patient with diabetes might need adjustments to their MS treatment to account for potential interactions.
Socioeconomic Factors and Access to Care
Socioeconomic factors, such as access to healthcare, insurance coverage, and transportation, can significantly impact a patient’s ability to adhere to treatment regimens and participate fully in assessments. Patients facing financial hardship may struggle to afford medication or transportation to appointments. Such factors can influence treatment outcomes and require proactive strategies for support. For example, telemedicine or mobile health programs can help overcome geographical barriers and improve access to care for patients in underserved communities.
Furthermore, providing financial assistance or flexible payment options can ease the burden on patients.
Culturally Sensitive Assessment Strategies
Cultural sensitivity is paramount in assessing MS treatment effectiveness. Different cultures may have varying perspectives on health, illness, and treatment, which can influence patient participation in assessments. Clinicians should be aware of these nuances and adapt their approach to ensure that the assessment process is culturally appropriate and respectful. This might involve using interpreters, incorporating culturally relevant health beliefs, or adjusting communication styles to ensure clear understanding.
Assessing multiple sclerosis (MS) treatment effectiveness involves looking at various factors, like symptom improvement and MRI scan results. While some treatments might seem promising, it’s crucial to critically evaluate all available information, including recent research findings. For example, researchers say IVF add-on treatments are ineffective, highlighting the importance of rigorous study design in determining true efficacy researchers say ivf add on treatments are ineffective.
Ultimately, a holistic approach considering patient response, side effects, and long-term outcomes is key to selecting the best MS treatment plan.
Addressing Disparities in Treatment Outcomes
Disparities in MS treatment outcomes exist across various demographics. These disparities often stem from a combination of socioeconomic factors, access to care, and cultural influences. To address these disparities, a multi-pronged approach is needed, focusing on equitable access to care, culturally sensitive assessment strategies, and tailored treatment plans. For instance, implementing culturally appropriate education programs and support groups can help improve patient understanding and adherence to treatment protocols.
Furthermore, fostering collaborative relationships with community health organizations and advocacy groups can enhance support systems for diverse populations.
Long-Term Treatment Management
Navigating multiple sclerosis (MS) requires a long-term commitment to treatment. Effective management extends far beyond the initial diagnosis and involves ongoing adjustments to treatment plans as symptoms evolve and individual needs change. This proactive approach ensures patients maintain optimal well-being and quality of life.Long-term MS treatment management is not a static process; it’s a dynamic journey that requires continuous monitoring, adaptation, and patient engagement.
The goal is to achieve the best possible outcomes by managing symptoms, slowing disease progression, and minimizing potential complications. This requires a collaborative effort between the patient, healthcare provider, and support network.
Strategies for Managing MS Treatment Long-Term
Effective long-term management hinges on a proactive and adaptable approach. Regular communication and collaboration between patients and healthcare providers are crucial. This includes open discussions about treatment goals, potential side effects, and lifestyle adjustments. Regular follow-up appointments allow for timely assessments and necessary modifications to the treatment plan.
Importance of Ongoing Monitoring and Adjustments
Ongoing monitoring is paramount to successful long-term MS management. Regular assessments of symptoms, disease activity, and treatment response allow for early detection of changes and timely interventions. This dynamic approach is essential for maintaining symptom control and slowing disease progression. Healthcare professionals must consider the individual patient’s response to treatment and adjust strategies as needed. This often involves a combination of medication adjustments, lifestyle modifications, and support strategies.
Factors Influencing Treatment Adherence
Several factors can impact a patient’s ability to adhere to their MS treatment plan. These include:
- Side effects of medications: Unpleasant side effects can significantly deter patients from adhering to their treatment regimen. Strategies to mitigate these side effects, such as adjusting medication dosages or exploring alternative therapies, can be crucial in maintaining adherence.
- Financial constraints: The cost of MS medications can be prohibitive for some patients. Navigating financial assistance programs, exploring affordable alternatives, or negotiating with insurance companies can alleviate these concerns and promote adherence.
- Lifestyle factors: Stress, sleep disturbances, and poor nutrition can negatively affect treatment adherence. Supporting patients in managing these lifestyle factors can greatly enhance their ability to maintain their treatment plan.
- Emotional factors: The emotional toll of living with MS can be substantial. Providing psychological support, connecting patients with support groups, and fostering a positive outlook can contribute to treatment adherence.
Strategies to Enhance Treatment Adherence
Improving treatment adherence requires a multifaceted approach. These strategies can be employed to enhance adherence:
- Open communication and education: Providing patients with clear and comprehensive information about their treatment plan, including potential side effects and benefits, empowers them to make informed decisions.
- Personalized treatment plans: Tailoring treatment strategies to individual needs and preferences can improve patient buy-in and increase adherence.
- Support systems: Connecting patients with support groups, family members, or friends can provide emotional support and practical assistance, encouraging them to remain committed to their treatment.
- Regular follow-up appointments: Regular check-ins with healthcare providers allow for addressing concerns, providing encouragement, and ensuring the treatment plan remains effective.
Sample Table: Treatment Adjustments
| Observed Change | Potential Treatment Adjustments |
|---|---|
| Increased fatigue and spasticity | Adjusting medication dosage, exploring alternative therapies (e.g., physical therapy, occupational therapy), and potentially introducing new medications. |
| Uncontrolled pain | Increasing pain medication dosage, exploring different types of pain management techniques, or adding a co-treatment approach. |
| Decreased cognitive function | Exploring cognitive rehabilitation programs, modifying lifestyle factors, or potentially considering new medication approaches. |
| Side effect intolerance | Adjusting medication dosage, exploring alternative therapies, or changing to a different medication. |
Visual Representation of Treatment Outcomes
Tracking MS symptom progression is crucial for evaluating treatment effectiveness. Visual representations, like graphs and charts, provide a clear and concise way to illustrate these changes over time, allowing for easier interpretation and communication of results. This method helps clinicians and patients better understand the impact of treatment decisions.
Visual Representation Types
Visual representations of MS treatment outcomes can take various forms, each with its own strengths. Line graphs are particularly useful for showcasing trends in symptom severity over time. Bar graphs can be used to compare the severity of specific symptoms before and after treatment. Scatter plots are effective for demonstrating the relationship between specific treatments and symptom improvement.
Choosing the appropriate graph type depends on the specific data being analyzed.
Creating Visual Representations in Software
Several software tools can facilitate the creation of effective visual representations of MS treatment outcomes. Microsoft Excel, Google Sheets, and specialized statistical software packages like R and SPSS are commonly used for this purpose.
- Microsoft Excel: Excel offers a user-friendly interface for creating basic graphs. Its built-in charting tools allow for customization of colors, labels, and legends. This software is suitable for simple data visualizations.
- Google Sheets: Google Sheets provides a similar functionality to Excel, allowing for real-time collaboration and data sharing. Its cloud-based nature makes it convenient for team-based analysis.
- R: R is a powerful programming language for statistical computing and graphics. It offers extensive customization options for creating complex visualizations and advanced statistical analyses. R is best suited for advanced data analysis and researchers.
- SPSS: SPSS is another statistical software package with advanced charting capabilities. It facilitates complex data manipulation and visualization for large datasets, particularly useful in research settings.
Example Data and Interpretation, How to assess ms treatment
Consider a hypothetical patient with relapsing-remitting MS. The following table demonstrates the progression of their Expanded Disability Status Scale (EDSS) score before and after a new treatment.
| Time Point | EDSS Score (Before Treatment) | EDSS Score (After 6 Months of Treatment) |
|---|---|---|
| Baseline | 2.5 | – |
| 3 Months | 3.0 | 2.8 |
| 6 Months | 3.5 | 2.6 |
| 9 Months | 4.0 | 2.4 |
A line graph displaying these data points would show a clear downward trend in the EDSS score after the treatment was initiated. This visual representation would demonstrate the potential positive impact of the treatment on disease progression.
Interpreting the Visual Representation
The interpretation of visual representations relies on careful consideration of the data presented. Key elements to consider include the baseline EDSS score, the rate of change in the score over time, and the consistency of the trend. Significant improvements in the EDSS score, as observed in the example, suggest a positive treatment response.
Common Side Effects and Management
Navigating MS treatment often involves weighing the benefits against potential side effects. Understanding these side effects and developing strategies for managing them is crucial for patient well-being and treatment adherence. This section delves into the common side effects associated with various MS treatments, offering practical management strategies and highlighting the importance of patient education.
Common Side Effects Across Treatments
A variety of side effects can occur, impacting patients in different ways. These can range from mild discomfort to more serious complications. Recognizing patterns and individual sensitivities is essential for proactive management.
- Fatigue: Many MS treatments can lead to increased fatigue, impacting daily activities and overall quality of life. This can be a common side effect across different treatment modalities. Strategies to manage fatigue often include lifestyle modifications like adequate sleep, regular exercise (when appropriate), and stress reduction techniques. For example, a patient might find that taking a short walk in the afternoon helps alleviate fatigue, or that practicing mindfulness exercises before bed improves sleep quality.
- Infections: Some treatments can weaken the immune system, increasing susceptibility to infections. This is particularly important to monitor, as infections can impact the course of MS and treatment efficacy. Maintaining good hygiene practices, getting sufficient rest, and promptly seeking medical attention for any signs of infection are essential.
- Gastrointestinal Issues: Digestive problems such as nausea, vomiting, or diarrhea can be side effects of certain MS treatments. Managing these issues often involves dietary adjustments, antiemetic medications (if prescribed), and maintaining hydration. For example, a patient might find that avoiding fatty foods or consuming smaller, more frequent meals helps alleviate nausea.
Side Effects Specific to Different Treatment Types
Different MS treatments have unique side effect profiles. This section Artikels some common side effects associated with specific treatment categories.
| Treatment Type | Potential Side Effects | Management Strategies |
|---|---|---|
| Disease-Modifying Therapies (DMTs) | Infections, flu-like symptoms, injection site reactions (for injectable DMTs), liver function abnormalities, blood clotting problems, fatigue. | Regular monitoring of blood work and infection symptoms. Adequate hydration, rest, and a balanced diet. Prompt reporting of any unusual symptoms. For injection site reactions, using a different injection site each time. |
| Immunosuppressants | Increased risk of infections, fatigue, hair loss, nausea, skin reactions, liver or kidney problems. | Regular monitoring of blood work and infection symptoms. Maintaining a healthy lifestyle, including a balanced diet and adequate sleep. Prompt reporting of unusual symptoms. |
| Symptomatic Medications | Drowsiness, dizziness, nausea, headaches. | Taking medications as prescribed, managing expectations regarding symptom relief. Adequate hydration and rest. |
Importance of Patient Education
Educating patients about potential side effects and their management strategies is paramount. This empowers them to actively participate in their treatment plan. Clear communication between patients and healthcare providers is essential. It also helps to foster a sense of shared responsibility for successful treatment outcomes. For instance, if a patient understands that certain side effects are common with a particular medication, they’re better prepared to recognize them and discuss them with their doctor.
This proactive approach ensures that the treatment is as effective and safe as possible.
Treatment Adherence and Patient Education
Staying committed to your multiple sclerosis (MS) treatment plan is crucial for managing the disease effectively. Consistent adherence significantly impacts disease progression and overall well-being. This often involves more than just taking medication; it encompasses understanding the treatment’s purpose, potential side effects, and lifestyle adjustments. A strong partnership between the patient and healthcare team is essential to optimize outcomes.
Importance of Patient Adherence
Consistent adherence to MS treatment regimens is vital for achieving and maintaining remission, slowing disease progression, and preventing long-term complications. Adherence directly impacts the effectiveness of treatments, leading to better clinical outcomes and improved quality of life. Studies consistently show a correlation between adherence and favorable treatment responses.
Strategies to Promote Patient Engagement
Effective communication and shared decision-making are key to fostering patient engagement. Clear explanations of the treatment regimen, including its rationale, potential benefits, and potential side effects, empower patients to actively participate in their care. Active listening, empathy, and tailoring information to individual needs are critical for building trust and rapport.
- Patient-centered approach: Healthcare providers should consider individual patient preferences, values, and cultural backgrounds when developing treatment plans and educational materials. This ensures that the information is relevant and accessible to the patient.
- Simplified language and visual aids: Complex medical terminology should be avoided in favor of clear, concise language. Visual aids such as diagrams, flowcharts, and videos can enhance comprehension and retention of information. These aids can make a significant impact on patient understanding.
- Regular follow-up appointments: Scheduled check-ins provide opportunities for addressing concerns, providing ongoing support, and reinforcing the importance of adherence. This helps maintain motivation and provides a platform for adjustments to the treatment plan as needed.
- Support groups and peer-to-peer programs: Sharing experiences with others facing similar challenges can provide emotional support, practical advice, and encouragement for maintaining adherence. Peer-to-peer support can significantly impact patients’ understanding of their condition and adherence to treatment.
Role of Patient Education
Patient education plays a pivotal role in empowering individuals to actively manage their MS. Providing comprehensive information about the disease, treatment options, and potential side effects equips patients with the knowledge to make informed decisions about their care. Well-informed patients are better positioned to adhere to their treatment plan and to advocate for their needs.
Examples of Educational Materials
A variety of educational resources can enhance patient understanding. These include:
- Brochures and pamphlets: These provide concise overviews of MS, treatment options, and potential side effects.
- Videos and online resources: Interactive videos and websites can explain complex information in an engaging and accessible manner. Online forums can be helpful for patients to connect and share experiences.
- Interactive tools and apps: Tools that track medication schedules, symptom logs, and treatment adherence can empower patients to actively monitor their progress and identify patterns.
- Educational workshops and seminars: Workshops provide a platform for interactive learning and address specific questions and concerns in a supportive environment. These workshops can be conducted by healthcare professionals or support groups.
Last Recap
In conclusion, assessing MS treatment requires a holistic approach that considers multiple factors. This guide has highlighted the importance of comprehensive assessment criteria, understanding diverse patient populations, and the long-term management strategies needed to achieve the best possible outcomes. By combining objective measurements with patient-centered care, we can navigate the complexities of MS treatment effectively. Remember, every patient’s experience is unique, and tailored assessments are crucial for successful management.