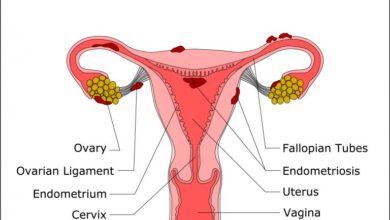
Endometriosis of fallopian tube, a condition where endometrial tissue grows outside the uterus, specifically affecting the fallopian tubes, presents a complex interplay of factors. This in-depth exploration delves into the intricacies of this condition, from its definition and causes to its impact on fertility and long-term management strategies. Understanding this unique form of endometriosis is crucial for both diagnosis and effective treatment.
This comprehensive guide covers the key aspects of fallopian tube endometriosis, including its varied symptoms, diagnostic procedures, available treatment options, and the crucial role it plays in fertility. We will examine the specific challenges posed by this condition, while also comparing it to general endometriosis, to gain a more complete picture of this intricate issue.
Definition and Overview
Endometriosis, a condition where tissue similar to the lining of the uterus (the endometrium) grows outside the uterus, can affect various organs, including the fallopian tubes. This often results in significant pain, fertility issues, and other complications. Understanding the specific ways endometriosis impacts the fallopian tubes is crucial for diagnosis and treatment.Endometriosis affecting the fallopian tubes, while part of the broader endometriosis condition, presents unique characteristics.
Unlike typical endometriosis, where endometrial implants are often found on the ovaries or pelvic peritoneum, fallopian tube involvement can lead to significant structural changes within the tubes. These changes can impact their function in transporting eggs and sperm. This localized involvement can have different implications for fertility and overall health.
Fallopian Tube Involvement in Endometriosis
Endometriosis in the fallopian tubes, often referred to as tubal endometriosis, involves the presence of endometrial tissue within the fallopian tubes. This can lead to a variety of manifestations, ranging from mild inflammation to significant scarring and blockage.
Dealing with endometriosis of the fallopian tubes can be tough, impacting everything from fertility to overall well-being. Sometimes, emotional struggles like those related to binge eating disorder can arise. Finding healthy coping mechanisms like meditation for binge eating disorder can be incredibly helpful in managing those emotions. Ultimately, though, focusing on managing the endometriosis itself is key to regaining control and improving quality of life.
Differences from Typical Endometriosis
Typical endometriosis is characterized by the presence of endometrial-like tissue outside the uterus, often in the pelvic region. However, fallopian tube involvement is unique because the endometrial tissue is situated within the fallopian tube itself. This can affect the structure and function of the tubes, leading to specific symptoms and complications.
Stages of Fallopian Tube Endometriosis
While a standardized staging system for fallopian tube endometriosis isn’t as well-defined as for ovarian endometriosis, the severity can be categorized based on the extent of the disease.
- Mild involvement: Characterized by small, superficial implants within the fallopian tubes, often accompanied by minimal inflammation. Symptoms may be mild or intermittent.
- Moderate involvement: Shows more extensive endometrial tissue growth, potentially causing some scarring or narrowing of the tubes. Symptoms are likely more pronounced and persistent, possibly impacting fertility.
- Severe involvement: Endometrial tissue significantly obstructs the fallopian tubes, leading to significant scarring, adhesions, and potential blockage. This stage often results in severe pain, infertility, and possible complications such as ectopic pregnancies.
Key Characteristics of Endometriosis in the Fallopian Tubes
The presence of endometrial implants in the fallopian tubes can manifest in several key ways.
Endometriosis affecting the fallopian tubes can be a real pain point, causing significant fertility issues. While the exact mechanisms behind this condition aren’t fully understood, researchers are actively exploring various avenues. Interestingly, some studies are looking at potential parallels between the immune response in endometriosis and how immunotherapy works against melanoma, how does immunotherapy work melanoma , which could lead to new diagnostic and treatment approaches for endometriosis of the fallopian tubes.
Further investigation is definitely needed in this area.
- Inflammation and pain: Endometrial tissue within the tubes can cause inflammation and pain, which can be cyclical or persistent. This pain may be felt during menstruation, sexual intercourse, or even during general activity.
- Scarring and adhesions: Endometrial implants can lead to scarring and adhesions within the fallopian tubes. This can cause the tubes to narrow or block, impacting the movement of eggs and sperm.
- Infertility: A common consequence of tubal endometriosis is infertility. The scarring and blockages can prevent the egg from reaching the uterus, or the sperm from reaching the egg.
- Ectopic pregnancy risk: Scarring and blockages within the fallopian tubes can create an environment where an egg may implant outside the uterus, increasing the risk of ectopic pregnancy. This is a serious complication requiring immediate medical attention.
- Dysmenorrhea: Painful menstruation, known as dysmenorrhea, is a frequently reported symptom of fallopian tube endometriosis, though its severity may vary depending on the stage of the condition.
Causes and Risk Factors
Understanding the causes and risk factors of endometriosis, particularly in the fallopian tubes, is crucial for diagnosis and treatment. While the exact cause remains elusive, a combination of genetic predisposition, hormonal influences, and environmental factors likely plays a role. This exploration delves into the potential triggers and associated risk factors, differentiating them from the general characteristics of endometriosis.The development of endometriosis, including its manifestation in the fallopian tubes, is a complex process involving multiple factors.
Research suggests a connection between genetic susceptibility and hormonal fluctuations in the body’s reproductive cycle. Environmental exposures and lifestyle choices may also contribute to the disease’s progression.
Potential Causes of Fallopian Tube Endometriosis
Several factors are implicated in the development of endometriosis affecting the fallopian tubes. These factors can include retrograde menstruation, where menstrual blood flows backward into the fallopian tubes, potentially carrying endometrial cells. Another proposed mechanism involves the transport of endometrial cells through the lymphatic system or blood vessels. Surgical procedures and hormonal imbalances can also potentially contribute to the condition.
Risk Factors for Fallopian Tube Endometriosis
Certain risk factors are associated with an increased likelihood of endometriosis impacting the fallopian tubes. These risk factors often overlap with general endometriosis but may present with unique characteristics.
- Retrograde Menstruation: This is a frequently cited potential cause, where menstrual blood containing endometrial cells flows backward into the fallopian tubes during menstruation. This phenomenon is thought to be a significant contributor to the development of endometriosis in general, and in the fallopian tubes specifically.
- Family History: A family history of endometriosis may increase the risk. This suggests a possible genetic predisposition to the condition, although the exact genes involved are not fully understood.
- Hormonal Factors: Fluctuations in estrogen levels, which are pivotal in regulating the menstrual cycle, are implicated in endometriosis. Elevated estrogen levels might promote the growth of endometrial cells outside the uterus, potentially impacting the fallopian tubes. This can be contrasted with general endometriosis where similar hormonal factors play a significant role.
- Previous Pelvic Surgery: Surgical procedures in the pelvic region, such as cesarean sections or appendectomies, might create a pathway for endometrial cells to implant in the fallopian tubes. This differs from general endometriosis, where the surgical history might not be a primary factor.
Comparison of Risk Factors with General Endometriosis
While many risk factors for general endometriosis are also relevant to fallopian tube endometriosis, some differences exist. For example, while retrograde menstruation is a significant factor in both, the specific pathways of endometrial cell implantation and growth might vary slightly in the fallopian tubes compared to other pelvic organs. Family history plays a role in both, suggesting a possible genetic predisposition, but the specific genes involved are not fully elucidated.
Furthermore, the influence of hormonal imbalances is also significant in both cases, but the specific hormonal triggers might differ.
Role of Genetics and Hormonal Factors
Genetic predisposition plays a crucial role in the development of endometriosis, potentially influencing the body’s response to hormonal changes. Research suggests that specific genes might make some individuals more susceptible to the condition. Further research is needed to fully elucidate the genetic mechanisms involved. Hormonal factors, particularly estrogen, are essential in regulating the menstrual cycle. Elevated estrogen levels might promote the growth of endometrial cells outside the uterus, potentially impacting the fallopian tubes.
This suggests a close relationship between hormonal fluctuations and the development of endometriosis.
Symptoms and Diagnosis
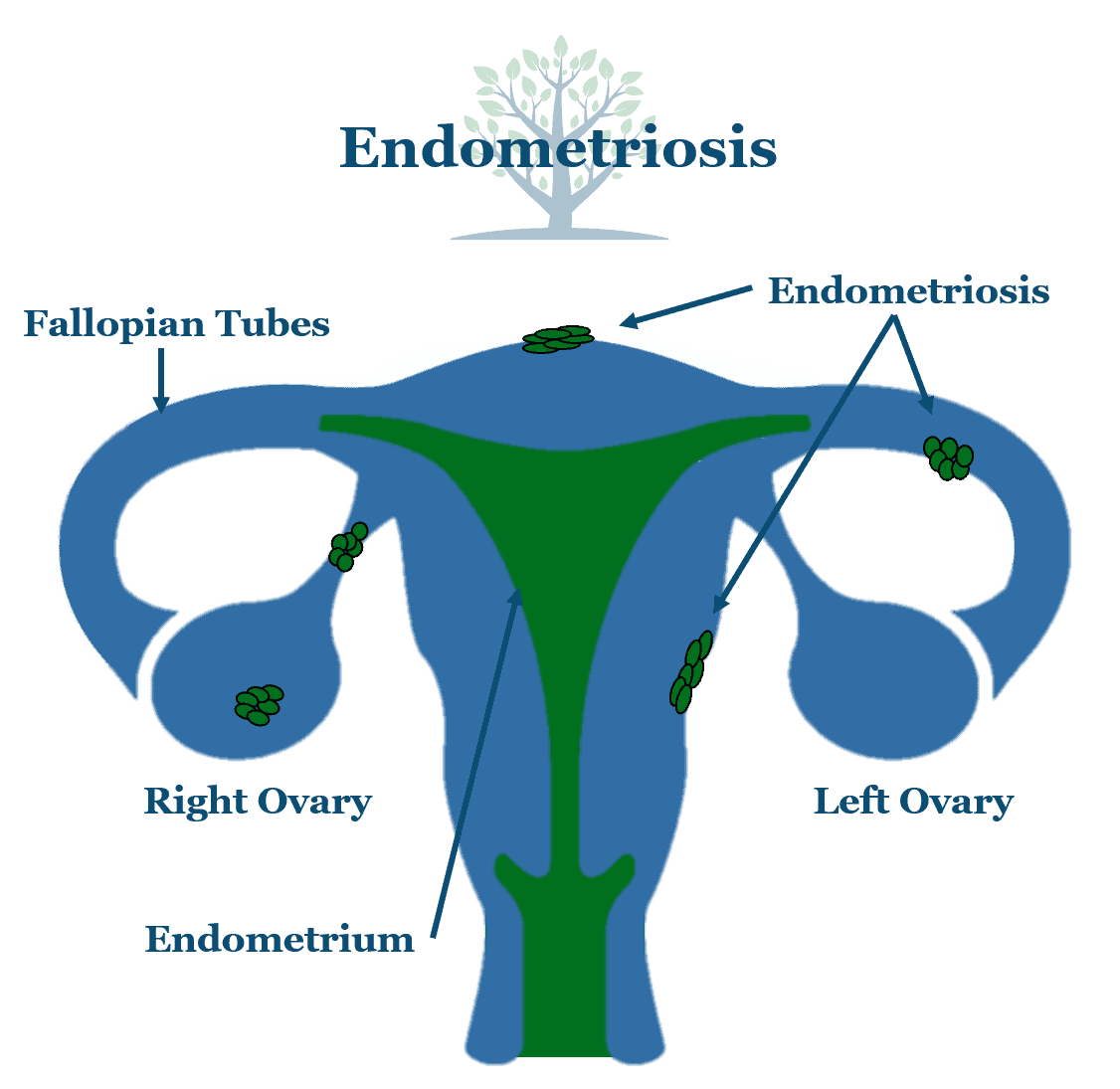
Navigating the complexities of endometriosis, particularly when it involves the fallopian tubes, can be challenging. Understanding the symptoms and diagnostic processes is crucial for early intervention and effective management. Early detection allows for timely treatment and potentially prevents complications.The symptoms of endometriosis affecting the fallopian tubes often mimic those of other conditions, making accurate diagnosis a crucial step.
This can sometimes lead to delays in proper treatment, potentially impacting fertility and overall well-being.
Common Symptoms
Recognizing the symptoms of endometriosis affecting the fallopian tubes is essential for timely diagnosis and treatment. These symptoms can vary in severity and presentation. They can sometimes be subtle, mimicking other conditions, which makes accurate diagnosis challenging.
- Pelvic pain, often described as cramping or sharp, is a prevalent symptom. This pain can worsen during menstruation, sexual intercourse, or bowel movements.
- Abnormal vaginal bleeding, such as heavy periods or bleeding between periods, can be another indicator.
- Painful or irregular bowel movements or urination can also be related symptoms.
- Infertility is a significant concern. Endometriosis affecting the fallopian tubes can block or damage the tubes, hindering the journey of the egg and sperm. This often manifests as difficulty conceiving or recurrent miscarriages.
- Symptoms can also include fatigue, bloating, nausea, and/or diarrhea. These symptoms are not specific to endometriosis of the fallopian tubes, and may arise from other conditions.
Potential Complications, Endometriosis of fallopian tube
Endometriosis in the fallopian tubes can lead to several complications. Understanding these complications can help prioritize the need for early diagnosis and treatment.
- Infertility: A major complication is the potential for infertility. Scar tissue and inflammation caused by endometriosis can obstruct the fallopian tubes, preventing the egg from reaching the sperm for fertilization.
- Ectopic Pregnancy: Damaged or scarred fallopian tubes can increase the risk of an ectopic pregnancy. An ectopic pregnancy occurs when the fertilized egg implants outside the uterus, typically in a fallopian tube. This is a serious condition that requires immediate medical attention.
- Chronic Pelvic Pain: The chronic inflammation and irritation caused by endometriosis can lead to persistent pelvic pain, affecting daily life and quality of living. This pain can be debilitating and significantly impact daily activities.
Diagnostic Methods
Accurate diagnosis of endometriosis affecting the fallopian tubes often involves a multi-faceted approach. This approach combines patient history, physical examination, and various diagnostic tests.
- Pelvic Exam: A physical examination of the pelvic area can reveal signs of tenderness or abnormalities suggestive of endometriosis.
- Imaging Techniques: Imaging plays a crucial role in diagnosing endometriosis in the fallopian tubes. Techniques include ultrasound, MRI, and laparoscopy.
- Ultrasound: Transvaginal ultrasound can help visualize the uterus and fallopian tubes. It can identify abnormalities in the fallopian tubes and surrounding structures, but may not always be sufficient for definitive diagnosis.
- MRI: Magnetic resonance imaging (MRI) provides detailed images of the pelvic organs. It can help visualize the extent of endometriosis and identify potential obstructions in the fallopian tubes.
- Laparoscopy: Laparoscopy is a minimally invasive surgical procedure that involves inserting a small camera into the abdomen. It allows direct visualization of the fallopian tubes and surrounding structures, providing a definitive diagnosis of endometriosis.
- Blood Tests: While blood tests alone cannot diagnose endometriosis, they can be helpful in ruling out other conditions. For example, elevated levels of certain hormones may be associated with endometriosis.
- Patient History: A thorough review of the patient’s medical history, including symptoms, menstrual cycles, and past surgeries, is essential for developing a comprehensive understanding of the condition and potential contributing factors.
Symptom Severity Table
The severity of symptoms can vary greatly between individuals. This table provides a general overview of potential symptoms and their corresponding severity levels.
| Symptom | Mild | Moderate | Severe |
|---|---|---|---|
| Pelvic Pain | Occasional, mild cramping | Frequent, moderate cramping, interfering with daily activities | Constant, severe pain, significantly impacting daily life |
| Abnormal Bleeding | Slightly heavier periods | Heavier periods, prolonged bleeding | Extremely heavy periods, bleeding between periods |
| Infertility | Difficulty conceiving, no pregnancy after trying for a short time | Significant difficulty conceiving, several unsuccessful attempts at conception | Unable to conceive after extended attempts |
Treatment Options
Navigating endometriosis in the fallopian tubes can feel overwhelming. Thankfully, various treatment options exist, each with its own set of benefits and drawbacks. Understanding these options is crucial for making informed decisions alongside your healthcare provider. Treatment strategies often depend on the severity of the condition, your overall health, and your desire for future fertility.
Surgical Approaches
Surgical interventions are frequently employed for endometriosis in the fallopian tubes. These procedures aim to remove the affected tissue and potentially restore normal fallopian tube function.
- Laparoscopic Surgery: This minimally invasive technique involves making small incisions to insert a tiny camera and surgical instruments. Laparoscopic surgery is often the preferred initial approach for endometriosis due to its reduced recovery time compared to open surgery. Surgeons can precisely target and remove affected tissue, minimizing damage to surrounding healthy tissue. However, the extent of the endometriosis and the surgeon’s experience can influence the effectiveness of this procedure.
- Open Surgery: In situations where laparoscopic surgery isn’t feasible or sufficient, open surgery may be necessary. This involves a larger incision, allowing for a more extensive view of the affected area. While open surgery offers a wider field of vision, it generally results in a longer recovery period compared to laparoscopic surgery. It’s usually reserved for cases with extensive or complex endometriosis.
Non-Surgical Management
Non-surgical treatment options for endometriosis in the fallopian tubes focus on managing symptoms and potentially slowing the progression of the disease. These methods are often used in conjunction with other treatments or as initial approaches before surgical intervention.
- Pain Management: Medications such as nonsteroidal anti-inflammatory drugs (NSAIDs) and over-the-counter pain relievers can help alleviate the pain associated with endometriosis. However, these medications may not address the underlying cause of the condition. More potent pain relievers, like opioids, might be considered for severe cases, but with careful consideration of potential side effects. Hormonal medications, like those used for birth control, can also help manage pain and potentially slow the growth of endometriosis.
- Hormonal Therapy: Hormonal therapies, such as combined oral contraceptives, progestin-only pills, or GnRH agonists, can reduce the amount of estrogen in the body. Lowering estrogen levels can help decrease the growth of endometrial tissue, thereby reducing pain and potentially preventing further spread. These therapies may have side effects, including mood changes, weight fluctuations, and vaginal bleeding irregularities.
Medication Role
Medications play a significant role in managing endometriosis in the fallopian tubes. They can help control symptoms, reduce inflammation, and potentially slow the progression of the disease. However, medications alone may not be sufficient for all cases, and surgical intervention may be required.
- NSAIDs: Nonsteroidal anti-inflammatory drugs, like ibuprofen and naproxen, can help alleviate pain and inflammation associated with endometriosis.
- Hormonal Contraceptives: Oral contraceptives, or other hormonal treatments, can help regulate hormonal cycles and potentially reduce the growth of endometrial tissue. Examples include birth control pills, progestin-only pills, and other hormonal therapies.
Treatment Comparison
The choice of treatment for endometriosis in the fallopian tubes depends on individual circumstances. A comprehensive evaluation of symptoms, severity, and future goals is crucial.
| Treatment Option | Pros | Cons |
|---|---|---|
| Laparoscopic Surgery | Minimally invasive, shorter recovery time, precise removal of affected tissue | Potential for recurrence, not suitable for all cases, risk of complications |
| Open Surgery | Provides wider surgical field, potentially removing more extensive endometriosis | Longer recovery time, greater risk of complications, larger incision |
| Pain Management | Relatively low cost, readily available | Limited effectiveness in addressing the underlying condition, may not manage severe pain |
| Hormonal Therapy | Potentially slows progression of endometriosis, manages symptoms | Side effects (e.g., mood changes, weight fluctuations), may not be effective for all individuals |
Impact on Fertility: Endometriosis Of Fallopian Tube
Endometriosis, when it involves the fallopian tubes, can significantly impact a woman’s ability to conceive naturally. The presence of endometrial tissue outside the uterus creates an inflammatory environment that can affect the delicate mechanics of the reproductive system, hindering the journey of an egg from the ovary to the uterus. This disruption can have various consequences for fertility, potentially impacting pregnancy rates and outcomes.Endometriosis in the fallopian tubes can lead to a range of complications that interfere with the normal process of fertilization and implantation.
These complications can be subtle, but their cumulative effect can make it challenging for a woman to achieve a pregnancy naturally. Understanding the specifics of this impact is crucial for appropriate management and treatment options.
Impact on Egg Transport
Endometrial tissue can obstruct or narrow the fallopian tubes, impeding the passage of the egg toward the uterus. This blockage can prevent fertilization from occurring, or even if fertilization happens, the resulting embryo may not be able to reach the uterus for implantation. Furthermore, the inflammatory response caused by endometriosis can create adhesions, which are fibrous bands that bind tissues together, potentially causing further blockages or distortions within the fallopian tubes.
These adhesions can distort the normal structure of the tubes, making it difficult for the egg and sperm to meet and for the fertilized egg to travel to the uterus.
Impact on Pregnancy Rates
Studies suggest a correlation between the severity of endometriosis and decreased pregnancy rates. Women with endometriosis in the fallopian tubes may experience lower rates of spontaneous pregnancy compared to women without the condition. The severity of the condition, the extent of the tubal involvement, and the presence of other factors like adhesions all contribute to the reduction in natural conception rates.
In some cases, the presence of endometriosis can significantly impact a woman’s ability to carry a pregnancy to term, potentially resulting in miscarriages or premature births.
Assisted Reproductive Technologies (ART)
In cases where natural conception is challenging or impossible due to endometriosis-related tubal issues, assisted reproductive technologies (ART) can be an option. These procedures aim to bypass the obstructed or damaged fallopian tubes to facilitate fertilization and implantation. Examples of ART include in vitro fertilization (IVF), where eggs are fertilized outside the body, and intracytoplasmic sperm injection (ICSI), where a single sperm is injected directly into an egg.
These methods allow for the selection of healthy embryos for transfer to the uterus, increasing the chances of successful implantation and pregnancy. Furthermore, careful consideration of endometriosis-related factors during ART procedures can significantly influence treatment success.
Potential for Future Pregnancies
The possibility of future pregnancies after treatment for endometriosis in the fallopian tubes varies depending on several factors. These factors include the severity of the condition, the extent of the tubal involvement, the type of treatment received, and the individual’s overall health. In some cases, treatment may restore the functionality of the fallopian tubes, allowing for successful natural conception in the future.
However, in other cases, ART may be necessary to achieve pregnancy. The long-term reproductive potential of a woman with endometriosis in the fallopian tubes is a complex interplay of these variables.
Connection to Tubal Infertility
Endometriosis can be a significant contributor to tubal infertility. The presence of endometrial implants and the inflammatory response in the fallopian tubes can cause damage and scarring, leading to blockages or impaired function. This damage can hinder the natural transport of the egg and sperm, reducing the chances of conception. The extent of tubal damage caused by endometriosis can vary, affecting the ability to conceive naturally or necessitate the use of assisted reproductive technologies.
Long-Term Management and Prevention
Living with endometriosis, particularly in the fallopian tubes, requires a proactive approach to long-term management. A personalized strategy, combining medical interventions with lifestyle adjustments, is crucial for minimizing symptoms and improving overall well-being. Regular check-ups and open communication with healthcare providers are essential for monitoring the condition and adapting treatment plans as needed.A comprehensive understanding of the condition’s potential impact on fertility and future reproductive plans is vital.
This requires careful consideration of long-term goals and a collaborative discussion with healthcare professionals.
Regular Check-ups and Follow-up Care
Regular check-ups are vital for monitoring the progression of endometriosis in the fallopian tubes. These visits provide opportunities to discuss any emerging symptoms, assess the effectiveness of current treatments, and make necessary adjustments. Follow-up care also allows for early detection of complications and proactive intervention. This proactive approach ensures that any potential problems are addressed promptly. It is crucial to maintain open communication with your healthcare provider, reporting any changes in symptoms, even seemingly minor ones.
This allows for timely intervention and prevents potential complications.
Lifestyle Modifications
Implementing lifestyle modifications can play a significant role in managing endometriosis and potentially reducing its impact. A balanced diet rich in fruits, vegetables, and whole grains, along with regular exercise, can contribute to overall health and well-being. Maintaining a healthy weight is also important, as obesity can exacerbate some symptoms.
Potential Preventative Measures
While there’s no definitive way to prevent endometriosis, certain lifestyle choices may help minimize the risk. Maintaining a healthy weight, consuming a balanced diet, and engaging in regular physical activity can contribute to overall health and well-being, which may indirectly reduce the risk of developing endometriosis. Smoking cessation is also important, as smoking has been linked to various health issues.
Dealing with endometriosis affecting the fallopian tubes can be tough, impacting fertility and overall well-being. It’s fascinating to consider how similar challenges might impact the immune system, like in cases of living with a chronic viral infection, which could age your immune system here. This raises important questions about potential long-term effects on the body’s ability to fight off infections, especially in the context of endometriosis and its ongoing impact on the reproductive system.
Recommendations for a Healthy Lifestyle
Adhering to a healthy lifestyle is crucial for women with a history of fallopian tube endometriosis. A balanced diet rich in fruits, vegetables, and whole grains, coupled with regular exercise, is beneficial. Maintaining a healthy weight and managing stress through relaxation techniques can also contribute to overall well-being.
- Prioritize a balanced diet: Focus on nutrient-rich foods, including fruits, vegetables, and whole grains. Limit processed foods, sugary drinks, and excessive saturated fats. This contributes to overall health and potentially reduces the risk of inflammatory conditions.
- Regular Exercise: Aim for at least 150 minutes of moderate-intensity aerobic activity per week. Exercise not only improves physical health but also helps manage stress, a factor that can influence endometriosis symptoms.
- Maintain a Healthy Weight: Maintaining a healthy weight is crucial. Obesity can exacerbate endometriosis symptoms. Consult with a healthcare professional or registered dietitian for personalized guidance.
- Manage Stress: Incorporate stress-reducing techniques such as yoga, meditation, or deep breathing exercises. Stress can impact hormone levels, which might influence the course of endometriosis.
- Quit Smoking: Smoking is linked to various health problems. Quitting smoking is beneficial for overall health and potentially reduces the risk of developing endometriosis.
Research and Future Directions
Unraveling the mysteries of endometriosis, particularly its impact on the fallopian tubes, requires ongoing research. Current studies are focusing on various aspects of the condition, from refining diagnostic tools to developing more effective and less invasive treatment options. This exploration promises to significantly improve the lives of those affected by this complex disease.Research into endometriosis is constantly evolving, driven by the need to understand the multifaceted nature of this condition.
Significant advancements are anticipated in the future, impacting diagnosis and treatment strategies. This progress will lead to more personalized approaches and improved patient outcomes.
Current Research Focuses
Research efforts are concentrated on understanding the underlying mechanisms driving endometriosis growth and progression in the fallopian tubes. This involves examining the role of genetic predisposition, hormonal influences, and immune responses. Researchers are also investigating the potential for novel biomarkers to aid in early and accurate diagnosis.
Potential Advancements in Diagnosis
Improved diagnostic tools are a key area of focus. Researchers are exploring the use of advanced imaging techniques, such as 3D ultrasound and magnetic resonance imaging (MRI), to enhance visualization of endometriosis lesions in the fallopian tubes. This may allow for earlier and more precise identification of the condition, leading to earlier intervention. Additionally, development of blood-based biomarkers, similar to those found in ovarian endometriosis, may enable non-invasive diagnostic methods.
These advancements could drastically improve the diagnostic process, particularly for early-stage cases.
Emerging Treatments and Therapies
Emerging therapies aim to target specific aspects of endometriosis development and progression. One promising area is the development of targeted drug therapies. These drugs may specifically inhibit the growth and spread of endometriosis lesions within the fallopian tubes. This approach, similar to current cancer treatments, may offer a more precise and effective method of managing the condition.
Furthermore, minimally invasive surgical techniques are being refined, allowing for more precise removal of lesions while minimizing potential damage to surrounding healthy tissue. This approach focuses on preserving fertility and reducing post-operative complications.
Areas Needing Further Research
Despite significant progress, certain areas require further investigation. The long-term effects of endometriosis on fallopian tube function and fertility remain poorly understood. Research is needed to fully understand the cumulative impact of endometriosis on reproductive health and devise strategies to mitigate these effects. Additionally, the development of effective preventative measures is an important area of study. Understanding the factors contributing to the development of endometriosis in the fallopian tubes could lead to the identification of potential preventative strategies.
Summary of Recent Studies
Recent studies have highlighted the importance of early diagnosis in managing endometriosis affecting the fallopian tubes. One study demonstrated a correlation between the severity of fallopian tube involvement and reduced fertility rates. Another study explored the potential of a new biomarker to identify patients at higher risk for developing endometriosis-related infertility. These studies emphasize the importance of proactive monitoring and treatment to preserve fertility.
Illustrations and Visual Aids
Visual representations are crucial for understanding the complex interplay of endometriosis and the fallopian tubes. These aids can help clarify the disease’s various stages, locations, and impact on fertility, providing a more accessible and intuitive understanding for patients and healthcare professionals. They allow us to visualize abstract concepts and facilitate a deeper comprehension of the intricate mechanisms involved.The following illustrations and diagrams provide a comprehensive visual representation of endometriosis within the fallopian tubes, detailing its progression and effects.
Fallopian Tube Anatomy and Endometriosis
A detailed diagram of the female reproductive system, highlighting the fallopian tubes, ovaries, uterus, and surrounding structures is essential. This illustration should clearly distinguish the normal anatomy of the fallopian tubes, their role in egg transport, and their connection to the uterus. Superimposed on this diagram, the location of endometriosis within the fallopian tubes should be clearly marked, showcasing potential sites of implantation and growth.
This visual aid emphasizes the anatomical context of endometriosis, highlighting its potential to affect the tube’s structure and function.
Stages of Endometriosis Development in Fallopian Tubes
This diagram should depict the progression of endometriosis in the fallopian tubes across different stages. Each stage should be illustrated with a clear, labeled image, indicating the level of endometrial tissue growth, potential adhesions, and the resulting distortion of the fallopian tube structure. The stages should visually demonstrate the progression from early implantations to advanced cases with significant scarring and tubal blockage.
Examples of these stages could include initial focal deposits, diffuse infiltration, and severe tubal distortion.
Treatment Options and Associated Risks
An infographic summarizing various treatment options for endometriosis of the fallopian tubes is beneficial. The infographic should visually present different treatment approaches, including surgical interventions (laparoscopic procedures, etc.) and medical therapies (hormonal medications). Each treatment option should be accompanied by a brief description and an assessment of its potential risks and benefits, such as potential complications, success rates, and side effects.
The infographic should use clear visual cues, such as icons or color-coding, to differentiate between the various treatment options.
Endometriosis Location in Fallopian Tubes
An image depicting the precise location of endometriosis within the fallopian tube is essential. This image should highlight the specific regions affected by the disease, such as the fimbriae (finger-like projections), the ampulla (widest part), or the isthmus (narrower part) of the fallopian tube. The image should clearly show the extent and depth of the endometrial implants within the fallopian tube wall, offering a visual representation of the disease’s spatial distribution.
The image should be labeled with clear anatomical references.
Impact of Endometriosis on Fallopian Tubes and Fertility
A schematic illustrating the impact of endometriosis on the fallopian tubes and its subsequent effect on fertility is crucial. This schematic should visually represent the ways in which endometriosis can cause tubal blockage, damage, or distortion, which in turn hinders the movement of eggs and sperm, reducing the chances of fertilization. The diagram should visually connect the presence of endometriosis with the potential for reduced fertility, and should include examples of how severe endometriosis can lead to infertility in some cases.
This visual aid helps in understanding the direct correlation between endometriosis, tubal function, and reproductive outcomes.
Final Summary
In conclusion, endometriosis of the fallopian tube is a significant reproductive health concern demanding meticulous attention. From its underlying causes to the diverse treatment approaches, and its profound impact on fertility, this condition requires a holistic understanding. This exploration offers a comprehensive overview, empowering individuals and healthcare providers to navigate the complexities of this condition with greater clarity and knowledge.
Further research and advancements in diagnosis and treatment are essential to improving the lives of those affected.