Diabetes care Joslin 100 years first human insulin shot marks a pivotal moment in medical history. Imagine a world without effective treatment for diabetes, a debilitating condition affecting millions. Before 1921, managing diabetes was a constant struggle, with severe symptoms and limited treatment options. The discovery and subsequent application of insulin at Joslin Diabetes Center revolutionized the lives of countless individuals, drastically improving their quality of life and paving the way for modern diabetes care.
This journey delves into the historical context, the discovery’s significance, and the enduring impact on society.
The Joslin Diabetes Center, founded in 1919, quickly became a leader in diabetes research. Early research at the Joslin Center focused on understanding the complex nature of diabetes and developing effective treatments. The center’s pioneering work contributed significantly to our understanding of the disease, impacting the development of new treatments and management strategies. This article highlights the pivotal role of Joslin in advancing diabetes care.
Historical Context of Diabetes Care
Before the groundbreaking discovery of insulin in 1921, diabetes was a devastating and largely incurable disease. Individuals with diabetes faced a bleak future, often marked by severe symptoms and a significantly shortened lifespan. Management strategies were limited, and the societal impact was profound, affecting individuals, families, and communities. This historical overview delves into the challenges and limitations of diabetes care prior to the insulin era.
Pre-1921 Diabetes Management Practices
Before the advent of insulin therapy, managing diabetes was a significant struggle. Treatment options were primarily focused on dietary restrictions and, in some cases, bloodletting. These approaches, while well-intentioned, were often ineffective and lacked scientific understanding of the disease’s underlying mechanisms.
Challenges and Limitations Faced by Those with Diabetes
Individuals with diabetes prior to 1921 faced numerous challenges. Severe symptoms like excessive thirst, frequent urination, and weight loss were debilitating. The lack of effective treatments meant that these symptoms often progressed, leading to complications such as kidney failure, blindness, and nerve damage. Early death was a common outcome. The pain and suffering associated with the disease significantly impacted their quality of life.
Societal Impact of Diabetes Before Insulin
Diabetes had a profound societal impact before insulin. Families were burdened by the costs associated with the disease and the care of individuals who were often bedridden or significantly incapacitated. The lack of effective treatments resulted in high mortality rates, impacting communities and the overall economy. The disease placed a substantial emotional and financial strain on individuals and society.
Early Symptoms and Diagnoses of Diabetes
Early diagnoses of diabetes often relied on observations of characteristic symptoms. Increased thirst, frequent urination, and unexplained weight loss were key indicators. However, the accuracy of diagnosis was often limited by the lack of sophisticated diagnostic tools. Early detection was crucial, but it was often challenging due to the limitations of medical knowledge.
Comparison of Pre-1921 Diabetes Treatments
| Treatment | Method | Effectiveness | Side Effects |
|---|---|---|---|
| Dietary Restrictions | Limited carbohydrate intake, specific food elimination | Variable; some individuals experienced temporary relief, but long-term effectiveness was limited. | Potential for malnutrition if not carefully managed. Strict adherence was difficult for many. |
| Bloodletting | Removal of blood to reduce “excess humors” | Ineffective and potentially harmful. It did not address the underlying metabolic imbalance. | Risk of infection, anemia, and shock. |
| Herbal Remedies | Use of various plant extracts | Generally ineffective and often lacked scientific backing. | Potential for adverse reactions and interactions with other treatments. |
| Exercise and Rest | Prescribed regimens | Some anecdotal evidence of modest improvement, but no conclusive evidence of effectiveness. | Potential for exacerbating symptoms if not properly managed. |
The Discovery of Insulin
The quest to understand and treat diabetes, a debilitating condition impacting millions, took a monumental leap forward with the discovery of insulin. This revolutionary hormone, crucial for regulating blood sugar levels, marked a turning point in the management of diabetes, drastically improving the lives of those affected. This pivotal moment in medical history stemmed from years of meticulous research and the combined efforts of brilliant minds.The discovery of insulin was a collaborative effort, building upon earlier research into the role of the pancreas in blood sugar regulation.
Early experiments in animals, and the observation of the effects of removing the pancreas, were crucial stepping stones. The identification of the specific hormone responsible for blood sugar control proved challenging, requiring persistent experimentation and meticulous analysis.
The Process and Key Individuals
The identification and isolation of insulin involved a painstaking process of scientific investigation. Early research focused on understanding the pancreas’s role in carbohydrate metabolism. Scientists like Oskar Minkowski and Josef von Mering played a pivotal role in demonstrating the link between pancreatic removal and the onset of diabetes in dogs. Their groundbreaking work laid the foundation for further research into the pancreatic hormone responsible for regulating blood sugar.
Further research by scientists like Frederick G. Banting and Charles Best, with crucial support from J.J.R. MacLeod, ultimately led to the isolation of insulin. Their meticulous experimentation and collaboration were critical to the success of the research.
Significance of the First Human Insulin Injection, Diabetes care joslin 100 years first human insulin shot
The first successful injection of insulin into a human patient marked a watershed moment in medical history. This injection, administered in 1922, was a testament to the scientific rigor and collaborative spirit that characterized the discovery process. It represented a radical shift from existing treatments, offering a tangible hope for those suffering from diabetes. This marked the beginning of a new era in the management of diabetes.
Ethical Considerations of Early Clinical Trials
The initial clinical trials of insulin, while groundbreaking, presented ethical challenges. Informed consent, a cornerstone of modern clinical research, was not as rigorously applied in the early 20th century. Access to the treatment was not uniform and there were significant disparities in the application of ethical standards. There were concerns about the safety and long-term effects of the treatment.
These ethical issues, while not fully addressed at the time, underscored the importance of ethical considerations in medical research, a principle that continues to guide modern practices.
Immediate Impact on Lives with Diabetes
The immediate impact of insulin on the lives of those with diabetes was nothing short of transformative. Before insulin, diabetes was often a death sentence, leading to debilitating complications and premature death. The ability to regulate blood sugar levels, achieved through insulin, dramatically altered this grim prognosis. It provided a chance at a more normal and productive life for individuals with diabetes.
Scientific Breakthroughs Paving the Way
The discovery of insulin was not an isolated event; it was built upon a foundation of previous scientific breakthroughs. These included the understanding of the pancreas’s role in carbohydrate metabolism, the development of laboratory techniques for isolating and purifying hormones, and the refinement of surgical procedures for animal experimentation. The accumulation of knowledge and meticulous experimental work was vital for the success of the insulin discovery.
Timeline of Key Events
| Date | Event | Significance |
|---|---|---|
| 1889 | Oskar Minkowski and Josef von Mering demonstrate the link between pancreatic removal and diabetes in dogs. | Fundamental step in understanding the role of the pancreas in blood sugar regulation. |
| 1921 | Frederick G. Banting and Charles Best begin research at the University of Toronto. | Formal research initiative aimed at isolating the pancreatic hormone. |
| 1922 | First successful injection of insulin into a human patient. | Landmark achievement, opening a new era in the treatment of diabetes. |
Joslin Diabetes Center and its Role

The Joslin Diabetes Center, a beacon of diabetes care for over a century, stands as a testament to human resilience and scientific progress. Its impact on the field is profound, shaping the way we understand, treat, and manage diabetes worldwide. From its humble beginnings to its current position as a global leader in diabetes research, the Joslin has consistently pushed the boundaries of knowledge and innovation.The Joslin Diabetes Center’s legacy is intricately woven into the fabric of modern diabetes care.
Its pioneering research and unwavering commitment to patient well-being have transformed the lives of millions affected by this chronic condition. The center’s contributions extend beyond clinical practice, encompassing cutting-edge research that continues to drive advancements in the field.
Founding and Early Years
The Joslin Diabetes Center was founded in 1916 by Dr. Elliott P. Joslin, a physician deeply committed to improving the lives of individuals with diabetes. Dr. Joslin recognized the significant unmet need for specialized care and dedicated his career to developing comprehensive approaches to diabetes management.
Initial efforts focused on patient education, rigorous monitoring, and the careful application of available treatments. This commitment to a holistic approach laid the foundation for the center’s future success.
Contributions to Diabetes Care
The Joslin Diabetes Center has consistently contributed to the evolution of diabetes care through various avenues. Its pioneering research has led to significant advancements in understanding the disease’s complexities, and the development of innovative therapies. This includes pioneering work on insulin administration, blood glucose monitoring, and the identification of risk factors associated with diabetes complications. The center’s contributions have been instrumental in improving outcomes for individuals with diabetes, reducing the incidence of long-term complications.
Key Figures and Their Impact
Several prominent figures have shaped the Joslin Diabetes Center’s trajectory and left an indelible mark on the field of diabetes care. Dr. Joslin himself, with his extensive clinical experience and dedication to patient care, established the center’s foundational principles. Subsequent generations of researchers and clinicians have built upon this foundation, continuing to advance our understanding of diabetes. Other notable figures include renowned endocrinologists who have played pivotal roles in research, education, and patient care at the center.
Joslin Diabetes Center’s 100 years of pioneering diabetes care, culminating in the first human insulin shot, is a testament to the power of medical breakthroughs. This incredible progress wouldn’t have been possible without the substantial investment from taxpayers, funding crucial research for drugs like insulin. Taxpayers fund research for drugs plays a vital role in enabling advancements in diabetes care, and the Joslin Center’s achievements stand as a powerful example of this partnership.
Impact on Diabetes Research
The Joslin Diabetes Center’s impact on diabetes research is undeniable. Its commitment to rigorous research has resulted in the publication of numerous influential articles and the development of innovative strategies for diabetes prevention and management. This research has fostered a deeper understanding of the disease’s mechanisms and has provided the basis for improved clinical guidelines and treatment options.
The center’s research has contributed significantly to the development of effective diabetes prevention strategies and the management of associated complications.
Joslin Diabetes Center’s 100 years of groundbreaking diabetes care, culminating in the first human insulin shot, is truly remarkable. However, managing chronic conditions like diabetes can sometimes lead to other health challenges, such as depression and rheumatoid arthritis flare-ups. Understanding the interplay between these conditions, like the complex interplay of insulin and glucose, is crucial for comprehensive care.
Learning more about the potential link between these issues can help improve overall well-being and inform treatment strategies. Ultimately, Joslin’s legacy in diabetes care reminds us of the importance of holistic health approaches, even in managing conditions beyond the initial breakthrough. Check out this article on depression and ra flare ups for more insights.
Biographies of Leading Figures
Dr. Elliott P. Joslin, the founder of the Joslin Diabetes Center, was a leading physician of his time. His dedication to diabetes care and his commitment to improving patient outcomes are exemplary. He authored several influential textbooks and made significant contributions to the understanding and treatment of diabetes.
Numerous other individuals have contributed to the Joslin’s success. They represent the dedication of researchers and clinicians committed to improving the lives of individuals affected by diabetes.
Major Research Areas and Accomplishments
| Research Area | Accomplishments | Key Researchers |
|---|---|---|
| Insulin Therapy and Administration | Development of improved insulin formulations and delivery methods, leading to better glucose control and reduced complications. | Various Joslin researchers |
| Diabetes Complications | Significant research into the mechanisms and prevention of long-term complications like nephropathy, retinopathy, and neuropathy. | Various Joslin researchers |
| Type 1 Diabetes | Studies on the pathogenesis, prevention, and treatment of type 1 diabetes, including investigation of islet cell transplantation. | Various Joslin researchers |
| Type 2 Diabetes | Research on the epidemiology, risk factors, and treatment of type 2 diabetes, including the development of lifestyle interventions and new drug therapies. | Various Joslin researchers |
| Diabetes Prevention | Development of effective strategies to prevent or delay the onset of diabetes, particularly focusing on lifestyle modifications. | Various Joslin researchers |
Impact of Insulin on Society
The discovery and widespread adoption of insulin marked a revolutionary turning point in the history of diabetes care. Before its introduction, diabetes was a devastating and often fatal condition. Patients faced a grim prognosis, characterized by significant limitations in daily life and a dramatically shortened lifespan. Insulin’s transformative impact on the lives of people with diabetes was immediate and profound, impacting not only individual health but also societal structures and expectations.The immediate impact of insulin on patients’ quality of life was nothing short of astonishing.
Previously, individuals with uncontrolled diabetes suffered from debilitating symptoms like frequent urination, excessive thirst, and persistent hunger. These symptoms often led to significant limitations in daily activities, affecting everything from work and school to social interactions. Insulin, by regulating blood sugar levels, alleviated these debilitating symptoms. Patients could now engage in more active lifestyles, participate more fully in social settings, and pursue educational and professional opportunities.
Imagine the liberation of being able to eat a meal without the fear of a severe blood sugar crash, or the joy of feeling energy instead of constant exhaustion.
Mortality Rates and Life Expectancy
The introduction of insulin led to a dramatic reduction in mortality rates and a substantial increase in life expectancy for people with diabetes. Before insulin, diabetes often resulted in death within a relatively short time. The ability to manage blood sugar levels through insulin therapy significantly reduced the risk of complications such as kidney failure, blindness, and heart disease.
Improved life expectancy enabled individuals to contribute more fully to society and experience the richness of a longer lifespan. For example, a person diagnosed with diabetes in the 1920s had a drastically reduced life expectancy compared to someone diagnosed with the same condition in the 1950s, thanks to advancements in insulin therapy.
Societal Views Towards Diabetes
Societal views toward diabetes also underwent a significant transformation after the advent of insulin. Prior to the discovery, diabetes was often shrouded in fear and misunderstanding. The devastating consequences of the disease were widely recognized, leading to social isolation and stigmatization of individuals with diabetes. The introduction of insulin began to shift this perception. As more people with diabetes thrived and led productive lives, societal understanding and acceptance grew.
This positive shift also encouraged increased research into diabetes and the development of more effective treatments.
Comparison of Experiences Before and After Insulin
The experiences of people with diabetes before and after insulin are vastly different. Before insulin, individuals with diabetes faced a relentless struggle against a debilitating illness. Their days were often filled with discomfort, restrictions, and the constant fear of complications. After insulin, the outlook shifted dramatically. Individuals gained a sense of control over their health, could pursue their passions, and experience a fuller range of life opportunities.
Imagine the difference between being confined to a life of severe limitations and having the freedom to participate fully in life’s experiences.
Role of Insulin in Societal Participation and Productivity
Insulin played a crucial role in enabling societal participation and productivity. Individuals with diabetes could now participate more fully in education, employment, and social activities. This increased participation had a ripple effect on society, enriching communities with diverse talents and perspectives. Before insulin, individuals with diabetes were often excluded from opportunities due to the limitations imposed by the disease.
Insulin, by improving their health and well-being, allowed them to fully contribute to society.
Improvements in Aspects of Life
| Aspect of Life | Before Insulin | After Insulin |
|---|---|---|
| Physical Health | Frequent debilitating symptoms, high risk of complications, shortened lifespan | Improved health outcomes, reduced risk of complications, increased lifespan |
| Social Participation | Limited social interactions due to illness, often isolated and stigmatized | Increased participation in social activities, reduced social isolation |
| Educational Opportunities | Restrictions on educational pursuits due to health limitations | Increased access to education and career advancement |
| Employment | Limited job opportunities due to health limitations | Increased employment opportunities and productivity |
| Overall Well-being | Constant struggle with symptoms and disease management | Increased quality of life and hope for a future |
Long-Term Effects and Modern Approaches
The initial discovery of insulin revolutionized diabetes care, but managing this chronic condition long-term presents unique challenges. Understanding the potential long-term effects and the innovative approaches to diabetes care today is crucial for individuals living with the disease and for healthcare professionals. This evolution includes a significant shift from simply managing blood glucose levels to comprehensive strategies encompassing lifestyle modifications, preventative measures, and the ever-increasing role of technology.The long-term effects of insulin use and management are multifaceted.
Sustained high blood sugar levels can lead to serious complications, including cardiovascular disease, nerve damage (neuropathy), kidney damage (nephropathy), and eye damage (retinopathy). Careful monitoring, adherence to treatment plans, and proactive lifestyle changes are vital in mitigating these risks.
Celebrating 100 years since the first human insulin shot at Joslin Diabetes Center is a huge milestone in diabetes care. It’s amazing to think about how far we’ve come, and how much better we understand this disease. Recently, I learned about a new hot tea honoring the insulin discoveries, new hot tea honors insulin discovers , which is a really cool tribute.
This certainly underscores the profound impact of that original Joslin achievement on the ongoing fight against diabetes.
Long-Term Effects of Insulin Therapy
Sustained high blood sugar levels can cause significant damage to various organs over time. Careful management is crucial to minimizing the long-term effects. This includes not only maintaining blood glucose levels but also managing other risk factors such as blood pressure, cholesterol, and weight. Early detection and aggressive treatment of complications are key to preserving quality of life and reducing the burden of the disease.
Advancements in Diabetes Care Since the Initial Injection
Since the initial insulin injection, diabetes care has undergone remarkable advancements. Early insulin therapy was often associated with significant side effects and required meticulous management. Modern treatments offer a wider range of insulin types, enabling more personalized approaches to blood glucose control. The understanding of the disease mechanisms has improved, leading to better prevention strategies and a more holistic approach to patient care.
Modern Approaches to Diabetes Prevention and Management
Modern approaches to diabetes prevention and management focus on a multifaceted strategy. Lifestyle interventions, including diet, exercise, and weight management, are crucial. Early diagnosis and intervention are vital for preventing complications. Continuous glucose monitoring (CGM) and insulin pumps provide enhanced control and flexibility.
Comparison of Treatments
Early 20th-century treatments for diabetes primarily involved dietary restrictions and, later, insulin injections. Modern treatments offer a broader range of insulin types, allowing for more precise dosage adjustments and personalized regimens. Lifestyle modifications, including regular exercise and a balanced diet, are integral to modern management strategies, playing a more prominent role than in the past. Technological advancements, such as continuous glucose monitors and insulin pumps, provide more accurate glucose readings and automated insulin delivery, dramatically improving patient outcomes.
Role of Technology in Modern Diabetes Care
Technology plays a significant role in modern diabetes care. Continuous glucose monitors (CGM) provide real-time glucose readings, enabling patients to adjust their insulin doses proactively. Insulin pumps automate insulin delivery, allowing for more flexible schedules and improved glucose control. Mobile health applications and telehealth services provide convenient access to information, support, and remote monitoring, which can improve adherence to treatment plans and improve quality of life.
Types of Insulin Available Today
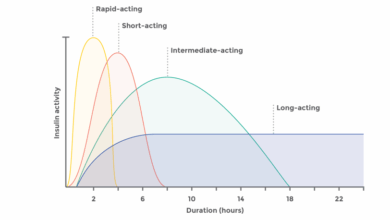
The diverse range of insulin types available today allows for greater flexibility and personalization in diabetes management. Different types of insulin vary in their onset, peak, and duration of action. This allows for customized regimens to suit individual needs and lifestyles.
| Type of Insulin | Action | Advantages/Disadvantages |
|---|---|---|
| Rapid-acting insulin | Rapid onset of action, typically within 15 minutes | Effective for controlling post-meal blood glucose spikes; requires careful timing with meals |
| Short-acting insulin | Onset within 30 minutes, peak in 2-4 hours, duration 5-8 hours | Effective for controlling post-meal blood glucose spikes; more predictable than rapid-acting, but requires more careful timing |
| Intermediate-acting insulin | Onset in 1-4 hours, peak in 4-12 hours, duration 16-24 hours | Provides basal insulin coverage; can be administered once or twice daily |
| Long-acting insulin | Slow and steady release, onset in 1-6 hours, no pronounced peak, duration 18-24 hours | Provides basal insulin coverage; can be administered once daily, reducing the risk of hypoglycemia between meals and overnight |
| Premixed insulin | Combination of short- or rapid-acting and intermediate-acting insulins | Convenience for those who prefer a single injection; may not be as flexible as using separate types |
Illustrative Historical Moments: Diabetes Care Joslin 100 Years First Human Insulin Shot
The discovery of insulin marked a pivotal moment in medical history, dramatically altering the lives of millions affected by diabetes. Understanding the atmosphere surrounding this groundbreaking event, the personal experiences of patients and families, and the reactions of the medical community paints a vivid picture of the transformative impact insulin had on society. This section delves into these illustrative historical moments, showcasing the human element behind this scientific triumph.
The Atmosphere Surrounding the First Insulin Injection
The air in the laboratory must have thrummed with a mix of anticipation and nervous energy. The potential for a life-saving breakthrough hung heavy in the air, mingling with the scent of antiseptic and the quiet hum of scientific instruments. The stakes were immense, as the fate of countless individuals with diabetes rested on the success of this groundbreaking procedure.
A Patient’s Experience with the First Insulin Injection
Imagine a patient, perhaps a young child or a frail adult, lying on a simple examination table. The room is likely dimly lit, filled with the quiet rustle of medical gowns and the soft murmur of conversation. The patient, likely experiencing the debilitating symptoms of untreated diabetes, would feel a slight prick as the first insulin injection was administered.
The immediate effects, though not fully understood, would likely be subtle, but significant. Perhaps there would be a slight sense of relief, a lessening of the severe symptoms, or a simple pause in the relentless progression of the disease. The patient would be entering a new chapter, one marked by hope and the potential for a better quality of life.
A Family Member’s Perspective
A family member witnessing the injection would likely be overwhelmed with a mix of emotions. Hope, fear, and an unfathomable relief would likely be intertwined. The relentless struggle to care for a loved one with uncontrolled diabetes would likely have taken a heavy toll. The first injection would mark the beginning of a new chapter, filled with uncertainty, yet with the profound hope for a healthier future.
They would likely be filled with gratitude and anticipation, observing closely for any signs of improvement in the patient’s condition.
The Medical Community’s Reaction
The medical community’s reaction to the discovery of insulin was one of cautious optimism and fervent collaboration. The early days would have been marked by intense research and experimentation to refine the dosage and administration techniques. Medical professionals, likely initially hesitant but compelled by the potential for a radical change in diabetes treatment, would have enthusiastically embraced the new technology.
Celebrating the 100th Anniversary of the First Human Insulin Shot
The 100th anniversary of the first human insulin shot would have been marked by a significant celebration, likely encompassing a range of activities from scientific symposiums and medical conferences to public awareness campaigns. The event would have been a testament to the transformative impact of the discovery, highlighting the enduring legacy of the pioneers who made it possible. This would have been an opportunity to recognize the progress made in diabetes care and to reflect on the journey that led to the current state of medical knowledge.
Public Perception of the Discovery
The public’s initial reaction to the discovery of insulin was likely one of awe and wonder. Newspapers and magazines would have carried articles detailing the breakthrough, showcasing the images of the groundbreaking researchers. The public would have been captivated by the narrative of scientific progress and the potential to alleviate suffering. This would have also highlighted the importance of medical research and the potential for scientific breakthroughs to improve the quality of life for people.
Ending Remarks

A century after the first human insulin injection, diabetes care has come a long way, thanks to the groundbreaking work at Joslin Diabetes Center. From rudimentary treatments to sophisticated management strategies, the impact of insulin on individuals’ lives and societal views of diabetes is undeniable. Today, advancements in technology and research continue to shape the future of diabetes care, with a focus on prevention and personalized treatment plans.
This journey through time underscores the transformative power of medical breakthroughs and the enduring commitment to improving the lives of those affected by this condition.