
Drug resistant superbugs are causing more deaths whats being done – Drug-resistant superbugs are causing more deaths, what’s being done? The rise of bacteria impervious to antibiotics poses a grave threat to global health. From the historical overuse of these life-saving drugs to the intricate mechanisms of bacterial resistance, this issue demands our urgent attention. We’ll explore the devastating impact on human health, the challenges in treatment, current strategies to combat this crisis, and the potential of emerging therapies.
The economic and social costs are immense, and we’ll delve into the preventive measures and future research directions needed to combat this escalating public health emergency.
This crisis demands a multifaceted approach, encompassing not only scientific innovation but also public health education and policy changes. We will examine the complex interplay between human actions, bacterial evolution, and the development of effective strategies to curb this threat. From the development of new antibiotics to promoting responsible antibiotic use, we will explore various perspectives on this global challenge.
Introduction to Drug-Resistant Superbugs
Drug-resistant superbugs, also known as antimicrobial-resistant bacteria, are a grave threat to global health. These are bacteria that have evolved to withstand the effects of antibiotics and other antimicrobial drugs, making them incredibly difficult to treat. This resistance poses a significant challenge to modern medicine, as infections caused by these superbugs can be far more serious and harder to manage than those caused by susceptible bacteria.Antibiotics, essential tools in fighting bacterial infections, have become less effective due to the overuse and misuse of these drugs.
The mechanisms by which bacteria develop resistance are complex and multifaceted, but they often involve genetic mutations that alter the bacteria’s structure or function, making them impervious to the drugs designed to kill them. This is a critical issue because it undermines the effectiveness of life-saving treatments.The global impact of antibiotic resistance is profound. Untreated infections caused by resistant bacteria can lead to prolonged illnesses, disability, and even death.
This issue disproportionately affects vulnerable populations, such as the elderly and those with compromised immune systems, and has a significant economic burden on healthcare systems worldwide. Furthermore, the lack of effective treatments hinders public health initiatives aimed at preventing and controlling infectious diseases.The historical context of antibiotic use plays a crucial role in the rise of superbugs. The widespread use of antibiotics in medicine, agriculture, and animal husbandry has created a selective pressure that favors the survival of antibiotic-resistant bacteria.
Over time, these resistant strains have multiplied, becoming a significant threat to human health. This underscores the importance of responsible antibiotic use and the development of new strategies to combat the problem.
Comparison of Drug-Resistant Bacteria
Understanding the diverse nature of drug-resistant bacteria is essential to developing effective strategies to combat them. The table below highlights various types of drug-resistant bacteria, their mechanisms of resistance, and the body systems they affect.
| Bacteria Type | Resistance Mechanism | Affected Body Systems | Examples of Infections |
|---|---|---|---|
| Methicillin-resistant Staphylococcus aureus (MRSA) | Produces enzymes that break down methicillin and other penicillin-like antibiotics. | Skin, lungs, bloodstream | Skin infections, pneumonia, bloodstream infections |
| Vancomycin-resistant Enterococci (VRE) | Modifications to cell wall components prevent vancomycin from binding effectively. | Gastrointestinal tract, urinary tract, bloodstream | Infections of the urinary tract, surgical site infections, bloodstream infections |
| Carbapenem-resistant Enterobacteriaceae (CRE) | Production of enzymes that break down carbapenems, a class of broad-spectrum antibiotics. | Gastrointestinal tract, urinary tract, bloodstream | Infections of the urinary tract, surgical site infections, bloodstream infections |
| Multidrug-resistant Tuberculosis (MDR-TB) | Mutations in genes involved in drug metabolism and transport, leading to resistance to multiple anti-TB drugs. | Respiratory system | Tuberculosis |
Impact of Drug-Resistant Superbugs
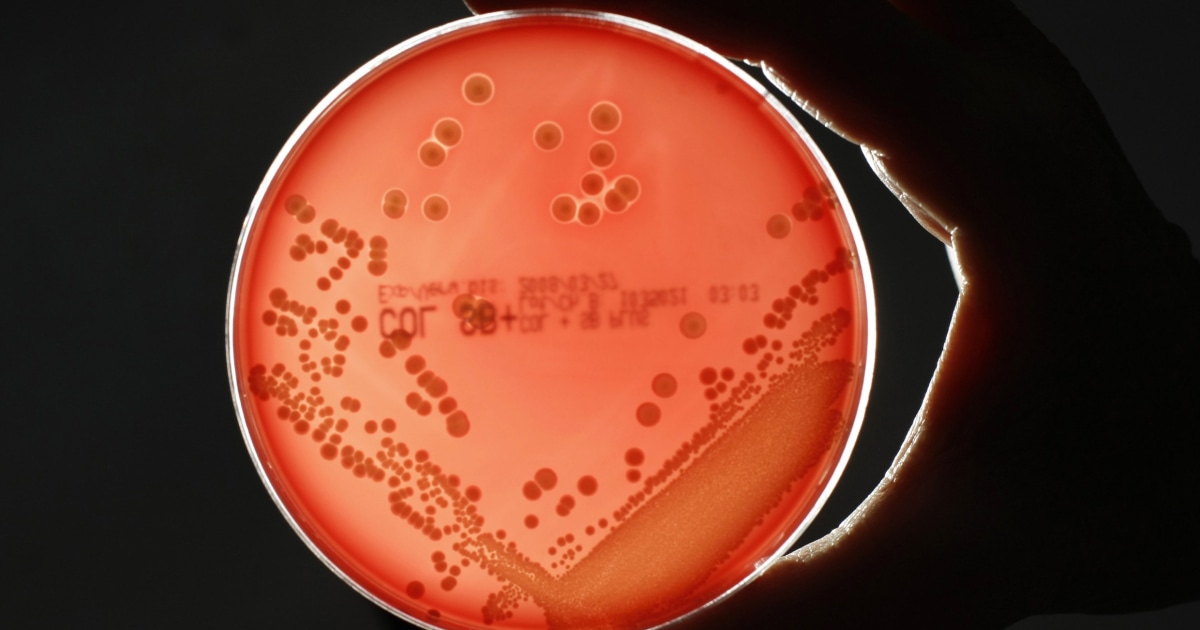
The rise of drug-resistant superbugs poses a significant threat to global health. These bacteria, no longer susceptible to the antibiotics that once effectively treated them, cause infections that are harder to control and often lead to more severe outcomes. This resistance has profound implications for individuals, healthcare systems, and public health as a whole.Untreated infections caused by drug-resistant bacteria can lead to a cascade of complications.
Severe infections can spread rapidly throughout the body, potentially causing organ damage or failure. The lack of effective treatment options can also prolong the suffering of patients, leading to prolonged hospital stays and reduced quality of life. For example, a simple skin infection in a patient with a compromised immune system can quickly escalate into a life-threatening bloodstream infection if antibiotic treatment is unavailable.
Consequences of Untreated Infections
The consequences of untreated infections caused by drug-resistant bacteria are often severe. Delayed or ineffective treatment can lead to sepsis, a life-threatening condition where the body’s response to infection damages its own tissues and organs. Infections may also spread to other parts of the body, creating more complex and challenging treatment scenarios. Further, complications can arise from the prolonged illness, including the development of chronic conditions or disabilities.
Challenges in Treating Patients with Superbug Infections
Treating patients with infections caused by drug-resistant bacteria presents significant challenges. Clinicians must employ a variety of diagnostic and therapeutic strategies to identify the specific resistant strain and find an effective treatment plan. This process can be time-consuming and expensive, requiring advanced laboratory tests and potentially experimental medications. Finding effective and suitable treatment options can be difficult, especially in cases of multi-drug resistant strains.
Mortality Rates Comparison
Mortality rates for infections caused by drug-sensitive bacteria are generally lower than those caused by drug-resistant bacteria. The ability to effectively treat infections with antibiotics significantly reduces the risk of death. In contrast, infections resistant to multiple antibiotics often result in higher mortality rates due to the limited treatment options available. For instance, a study on pneumonia cases showed a significantly higher death rate in patients infected with drug-resistant strains compared to those infected with drug-sensitive strains.
Economic Burden of Drug-Resistant Infections
Drug-resistant infections place a substantial economic burden on healthcare systems. The increased costs associated with treatment, including prolonged hospital stays, specialized care, and experimental medications, strain resources. This burden extends beyond direct healthcare costs, impacting productivity and economic losses from lost workdays and decreased quality of life. For example, a prolonged hospital stay due to a drug-resistant infection can lead to substantial economic losses for both the patient and the healthcare system.
Costs Associated with Treating Drug-Resistant Infections
| Infection Type | Hospitalization Costs (USD) | Medication Costs (USD) | Long-Term Care Costs (USD) |
|---|---|---|---|
| Methicillin-resistant Staphylococcus aureus (MRSA) Pneumonia | 15,000-30,000 | 2,000-5,000 | 5,000-10,000 |
| Vancomycin-resistant Enterococcus faecium (VRE) Bloodstream Infection | 20,000-40,000 | 3,000-8,000 | 10,000-20,000 |
| Carbapenem-resistant Enterobacteriaceae (CRE) Urinary Tract Infection | 12,000-25,000 | 1,500-4,000 | 4,000-8,000 |
Note: These costs are estimates and can vary significantly depending on factors such as the severity of the infection, the location of care, and the specific treatment required.
Current Strategies to Combat Drug Resistance
The rise of drug-resistant superbugs poses a significant threat to global health. These bacteria, capable of evading the effects of antibiotics, demand urgent and multifaceted strategies to combat their spread and impact. Effective strategies are crucial for maintaining the effectiveness of existing treatments and preventing a future where even common infections become untreatable.The fight against drug-resistant superbugs requires a coordinated effort involving multiple stakeholders, from researchers and healthcare providers to governments and individuals.
This includes bolstering research and development to create new antibiotics, promoting responsible antibiotic use, and improving infection control protocols in healthcare settings. These strategies are not isolated but rather interconnected, each playing a vital role in containing the spread of these dangerous pathogens.
Research and Development of New Antibiotics
A critical component of combating drug resistance is the development of new antibiotics. Existing antibiotics are losing their effectiveness as bacteria evolve resistance mechanisms. This necessitates continuous investment in research and development to discover novel antibacterial agents. The process of developing new antibiotics is complex and lengthy, often facing significant financial and logistical hurdles. However, successful outcomes offer hope in preserving the effectiveness of current treatments and combating future outbreaks.
Responsible Antibiotic Use
Inappropriate and excessive antibiotic use is a major driver of drug resistance. Patients need to understand the importance of only taking antibiotics when prescribed by a healthcare professional and completing the entire course as directed. Overuse in agriculture and animal husbandry also contributes to the problem. Strategies to promote responsible antibiotic use must target both healthcare providers and the public to minimize unnecessary prescriptions and ensure that antibiotics are used effectively when necessary.
Improving Infection Control in Healthcare Settings
Hospitals and other healthcare facilities are often hotbeds for the emergence and spread of drug-resistant bacteria. Strict adherence to infection control protocols is paramount. These protocols include hand hygiene, proper sterilization of equipment, and isolation procedures for infected patients. Proactive measures, such as environmental disinfection and screening for resistant pathogens, are vital for preventing the spread of these organisms.
Country-Specific Initiatives to Combat Antibiotic Resistance
| Country | Legislation | Awareness Campaigns | Research Funding |
|---|---|---|---|
| United States | Antimicrobial Stewardship Programs (ASPs) are increasingly implemented to improve antibiotic prescribing practices. | Public awareness campaigns highlight the importance of responsible antibiotic use. | Significant funding is allocated to research institutions for developing new antibiotics and studying resistance mechanisms. |
| United Kingdom | Stringent regulations govern the use of antibiotics in livestock farming to minimize resistance development. | Educational materials and campaigns target healthcare professionals and the public. | Government funding supports research projects focusing on new treatment strategies and infection control. |
| Canada | Legislation is being reviewed and updated to address the misuse of antibiotics. | Educational initiatives focus on proper hygiene practices in healthcare settings. | Research funding is directed toward identifying and developing new antibiotics. |
| Germany | Regulations are in place to control antibiotic use in animal feed. | Public awareness campaigns emphasize the need for responsible use of antibiotics. | Significant investments in research are geared toward understanding and mitigating resistance. |
The table above provides a glimpse into the diverse approaches countries are taking to combat antibiotic resistance. Each nation’s strategy reflects its unique challenges and priorities. The shared goal remains to curtail the alarming rise of these superbugs.
The rising threat of drug-resistant superbugs is a serious global concern, and the world is scrambling to find solutions. While scientists race to develop new antibiotics, the recent Netflix show on anorexia, which has sparked a fascinating debate ( netflix show on anorexia sparks debate ), highlights the complex interplay between public health crises and societal discussions. Ultimately, both the fight against superbugs and the ongoing conversations about mental health issues like anorexia underscore the need for comprehensive strategies to tackle health challenges on multiple fronts.
Emerging Treatments and Therapies
The relentless rise of drug-resistant superbugs necessitates a radical shift in our approach to infection control. Traditional antibiotics, once a cornerstone of modern medicine, are increasingly ineffective against these formidable pathogens. Consequently, innovative therapies and treatments are being actively explored to combat this growing threat. These emerging strategies offer a glimmer of hope, but also present unique challenges that must be addressed to ensure their efficacy and safety.New avenues of treatment are being explored, including phage therapy, antimicrobial peptides, and novel antibiotic development.
Each approach presents unique mechanisms of action and potential advantages, but also faces hurdles in terms of clinical translation and long-term safety. Understanding the strengths and weaknesses of these emerging treatments is critical to developing effective strategies to combat drug-resistant infections.
The rise of drug-resistant superbugs is a serious global health concern, and sadly, more people are dying from them. Luckily, initiatives like the ones in Howaa City, detailed in their fantastic report on howaa city gets healthy , offer valuable insights into preventative measures. Focusing on community health and education, like Howaa City’s approach, could provide important solutions to combat the spread of these dangerous infections and save lives.
Novel Antibiotic Development
The process of developing new antibiotics is a lengthy and complex undertaking. It often involves years of research and rigorous testing to ensure safety and efficacy. A comprehensive understanding of bacterial mechanisms, combined with innovative chemical synthesis, is crucial to the discovery of novel antibiotic compounds.
- Initial Research and Target Identification: The initial stage involves identifying specific bacterial targets within the pathogen. This is often done through meticulous study of bacterial processes like protein synthesis, cell wall formation, or DNA replication. Scientists aim to find vulnerable points in the bacteria that can be exploited without harming human cells. For instance, targeting enzymes unique to bacterial metabolism can lead to highly effective and specific antibiotics.
- Chemical Synthesis and Optimization: Once a target is identified, scientists synthesize potential antibiotic compounds. This process often involves extensive experimentation to fine-tune the chemical structure of the compound, optimizing its effectiveness and reducing toxicity. Computer modeling plays a vital role in predicting the behavior of new molecules and streamlining the design process.
- Preclinical Testing: Thorough preclinical testing is essential to evaluate the safety and efficacy of potential new antibiotics. This involves a series of laboratory experiments and animal studies. The tests measure the compound’s ability to inhibit bacterial growth, its toxicity to human cells, and its pharmacokinetic properties, such as absorption, distribution, metabolism, and excretion.
- Clinical Trials: Successful preclinical testing leads to clinical trials, which are conducted on human volunteers to further assess the safety and efficacy of the antibiotic. These trials involve various phases, from testing on a small group of patients to large-scale trials to confirm effectiveness and establish the optimal dosage. This process helps identify potential side effects and further refine the compound’s application.
Phage Therapy
Bacteriophages, or phages, are viruses that specifically infect and destroy bacteria. Phage therapy harnesses this natural phenomenon to combat bacterial infections. The approach leverages the phage’s ability to target and eliminate specific bacterial strains, potentially minimizing collateral damage to the host.
- Mechanism of Action: Phages attach to bacterial cells, inject their genetic material, and replicate within the bacteria. This replication process ultimately leads to the destruction of the bacterial cell. The process is highly specific, as phages only infect and replicate within specific bacterial species, minimizing harm to the host.
- Advantages: Phage therapy offers the potential for highly targeted bacterial elimination, and because they evolved to infect bacteria, they often exhibit greater resistance to bacterial resistance mechanisms compared to traditional antibiotics. The reuse of phages could be a sustainable solution to combatting superbugs.
- Challenges: Developing and implementing phage therapy strategies presents challenges, including the identification of appropriate phages for specific bacterial strains, ensuring their stability and safety for human use, and potential for phage inactivation or bacterial resistance.
Antimicrobial Peptides
Antimicrobial peptides (AMPs) are short chains of amino acids that exhibit potent antibacterial activity. They often target bacterial cell membranes, disrupting their structure and leading to cell death.
- Mechanism of Action: AMPs disrupt bacterial cell membranes by binding to and inserting themselves into the membrane. This process causes membrane permeabilization, leading to leakage of essential cellular components and bacterial cell death.
- Advantages: AMPs often exhibit broad-spectrum activity against various bacterial species, including those resistant to traditional antibiotics. Some AMPs also exhibit antiviral activity, which could potentially lead to wider applications in infection control.
- Challenges: The development of AMPs for clinical use is hindered by their potential toxicity to human cells and the difficulty in producing them on a large scale at a low cost.
Prevention and Public Health Measures
The escalating threat of drug-resistant superbugs necessitates a multifaceted approach that goes beyond treatment. Proactive measures focusing on prevention and responsible use of antibiotics are crucial to stem the tide of these dangerous infections. By altering individual and societal behaviors, we can significantly reduce the spread of these resistant pathogens and safeguard public health.Preventing the emergence and spread of drug-resistant infections requires a concerted effort to reduce the selection pressure for resistance.
This involves a combination of strategies, from promoting vaccination to educating the public about responsible antibiotic use. A comprehensive approach is vital to achieving lasting impact.
Preventive Measures to Reduce Spread
Effective preventive measures are critical in reducing the spread of drug-resistant infections. These measures encompass various strategies aimed at minimizing the conditions that favor the development and transmission of resistant pathogens. Hygiene practices, including handwashing, are paramount in preventing the spread of infectious agents. Proper food handling and sanitation practices further limit the exposure to potential sources of infection.
Importance of Vaccination
Vaccination plays a significant role in preventing bacterial infections. Vaccines stimulate the immune system to develop immunity against specific bacterial strains, thereby reducing the risk of infection. Immunization not only protects the vaccinated individual but also contributes to herd immunity, safeguarding those who cannot be vaccinated. The efficacy of vaccines in preventing bacterial infections has been extensively demonstrated.
For example, the widespread use of the pneumococcal vaccine has significantly reduced the incidence of pneumococcal pneumonia.
It’s terrifying how drug-resistant superbugs are increasing death tolls, and researchers are scrambling to find solutions. Meanwhile, interesting new research suggests that psoriasis medication Otezla might be linked to weight loss in people with psoriatic arthritis, according to a recent study ( psoriasis medication otezla leads to fat loss in people with psoriatic arthritis study says ). This could potentially offer a new avenue for treating related conditions, but it’s still early days, and we need more research to fully understand the implications for the fight against superbugs.
Strategies for Promoting Responsible Antibiotic Use
Responsible antibiotic use is paramount in curbing the development of drug resistance. Promoting awareness among both the public and healthcare professionals is essential to ensure appropriate antibiotic prescriptions and usage. The overuse and misuse of antibiotics create selective pressure for bacteria to develop resistance. By promoting responsible antibiotic use, we can limit this pressure and preserve the efficacy of these essential drugs.
Public Health Campaigns for Responsible Antibiotic Use
Public health campaigns play a critical role in educating the public about responsible antibiotic use. These campaigns should encompass a variety of strategies, including educational materials, targeted advertising, and community engagement. These campaigns should emphasize the importance of seeking medical advice before taking antibiotics and completing the full course of antibiotics as prescribed. This will ensure that the treatment is effective and that the bacteria are not allowed to develop resistance.
| Campaign Component | Educational Materials | Targeted Advertising | Community Engagement |
|---|---|---|---|
| Goal | Provide clear and concise information about antibiotic resistance and responsible use. | Reach specific demographics through targeted messaging. | Involve the community in the campaign through workshops, events, and community outreach. |
| Examples | Brochures, pamphlets, posters, videos, and websites with information about antibiotic resistance and responsible use. | Television and radio ads, social media campaigns, and targeted print advertisements. | Community health fairs, school presentations, workshops for healthcare professionals, and partnerships with community organizations. |
| Target Audience | General public, healthcare professionals, and patients. | Specific age groups, socioeconomic backgrounds, and geographic locations. | Individuals, families, and community groups. |
| Evaluation Metrics | Tracking the number of downloads, views, and interactions with educational materials. | Measuring the reach and impact of advertisements through surveys and focus groups. | Gathering feedback from community members and evaluating the participation in community events. |
Future Directions and Research

The fight against drug-resistant superbugs demands innovative and multifaceted approaches. Future research must prioritize understanding the intricate mechanisms of resistance, developing novel therapies, and implementing strategies to prevent the emergence of new resistant strains. This requires a collaborative effort across disciplines, from microbiology and pharmacology to engineering and public health.
Novel Therapeutic Strategies
Developing entirely new classes of antibiotics is crucial. Current efforts focus on targeting different pathways of bacterial metabolism, inhibiting specific enzymes, or disrupting essential cellular processes. For example, bacteriophages, viruses that infect bacteria, are being explored as a potential therapeutic approach. They can selectively target and kill bacteria without harming human cells. Moreover, research into inhibiting bacterial biofilm formation is vital.
Biofilms protect bacteria from antibiotics, making them more resistant. New approaches targeting these biofilms are emerging as promising avenues.
Improving Diagnostics and Surveillance
Early detection and rapid identification of drug-resistant bacteria are essential for effective treatment and containment. Advanced diagnostic tools, such as rapid molecular tests, can provide quicker results compared to traditional methods. These rapid tests allow for faster treatment decisions and limit the spread of infections. Furthermore, robust surveillance systems are necessary to track the emergence and spread of resistance patterns in different geographical locations.
This data is critical for informing public health interventions and guiding research priorities.
Developing Combination Therapies
Combining different antibiotics or antibiotic-like compounds may be a powerful strategy to combat drug resistance. The synergistic effect of combining agents could inhibit the growth of bacteria more effectively than individual treatments. For example, pairing a bacteriophage with a conventional antibiotic could enhance the efficacy of both. This approach has the potential to delay the emergence of resistance mechanisms and improve treatment outcomes.
Exploring Alternative Approaches
Beyond antibiotics, alternative approaches like bacteriophages and antimicrobial peptides are gaining traction. Bacteriophages can specifically target and eliminate bacteria without causing significant collateral damage to human cells. Antimicrobial peptides, produced naturally by the immune system, are another promising avenue. Further research into their efficacy and potential applications is necessary. Additionally, exploring new targets for inhibiting bacterial growth, such as quorum sensing molecules, could provide novel avenues for combating drug resistance.
Table: Comparing Research Approaches, Drug resistant superbugs are causing more deaths whats being done
| Research Approach | Strengths | Weaknesses | Potential Outcomes |
|---|---|---|---|
| Bacteriophage therapy | Highly specific to bacteria, potentially less resistance development | Potential for unknown side effects, requires isolation and characterization of specific phages for each pathogen | Effective treatment of infections, especially in combination with antibiotics |
| Antimicrobial peptides | Natural origin, potentially less resistance development, wide range of applications | Limited potency, potential for toxicity in high concentrations | Novel therapeutic options, particularly for wound infections |
| Combination therapies | Potentially greater efficacy, slower resistance development | Increased complexity in administration, potential for adverse drug interactions | Improved treatment outcomes, delays resistance emergence |
| Novel antibiotics | Targeted approach, potential for higher efficacy | High cost and time investment in development, potential for unforeseen resistance | New classes of effective drugs, delays resistance |
Interdisciplinary Collaboration
Tackling the antibiotic resistance crisis requires a concerted effort from various scientific disciplines. Microbiologists, pharmacologists, chemists, engineers, and public health experts need to collaborate to share knowledge, resources, and expertise. Joint research projects can accelerate progress and lead to more comprehensive solutions. Such collaboration is vital for tackling this global health challenge effectively.
Final Review: Drug Resistant Superbugs Are Causing More Deaths Whats Being Done
In conclusion, the growing threat of drug-resistant superbugs demands immediate and concerted action. The discussion highlights the urgent need for a multi-pronged approach, involving innovative research, responsible antibiotic use, and enhanced public health measures. The future hinges on our collective commitment to combating this escalating crisis. Continued research and global collaboration are essential to prevent the worst-case scenarios, ensuring effective treatments and safeguarding future generations from the devastating impact of these superbugs.
